New Study Demonstrates Potential for a Gene Therapy for Vanishing White Matter Disease
New Study Demonstrates Potential for a Gene Therapy for Vanishing White Matter Disease https://pediatricsnationwide.org/wp-content/uploads/2024/06/Bradbury-Vanishing-White-Matter-Image-1024x552.jpg 1024 552 Katie Brind'Amour, PhD, MS, CHES Katie Brind'Amour, PhD, MS, CHES https://pediatricsnationwide.org/wp-content/uploads/2021/03/Katie-B-portrait.gif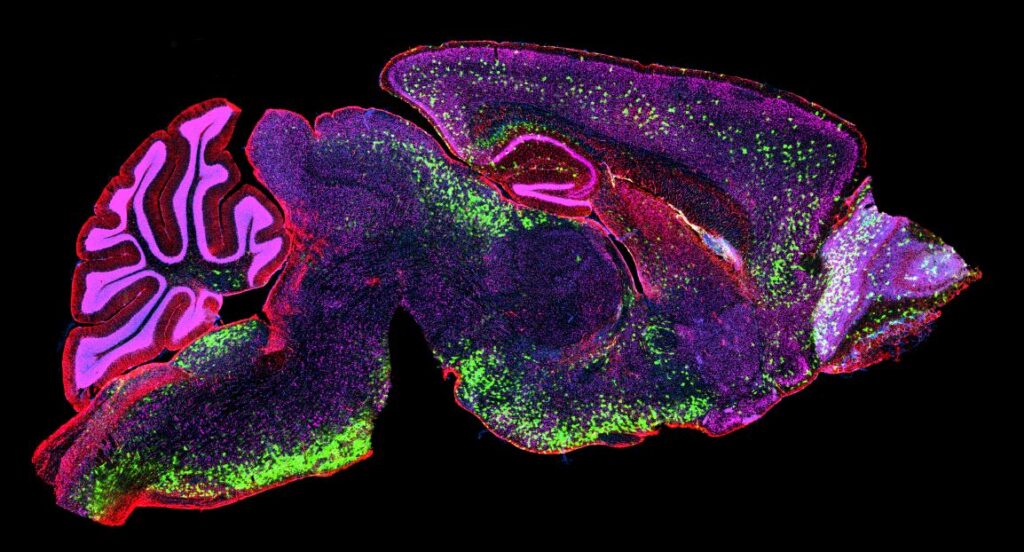
The research, conducted in mouse models, shows promising safety and efficacy for a currently incurable, life-limiting condition.
Researchers at Nationwide Children’s Hospital have confirmed initial safety and efficacy data for a gene supplementation therapy for Vanishing White Matter (VWM) disease in mouse models. Testing multiple versions of therapy in two separate mouse models representing different severity levels of the disease, the research team has demonstrated that their approach targets the right type of brain cells and rescues function in gait, motor function and body weight while attenuating demyelination and extending survival.
The results come after disappointing results from gene editing studies at other institutions suggesting that VWM disease was not amenable to genetic treatment, and concern from the genetic research community that diseases such as VWM may not respond well to therapies delivered through viral particles, such as the common gene therapy carrier known as adeno-associated virus, or AAV.
Vanishing White Matter disease is so named due to the sudden onset of neurodegeneration following an infection, trauma or other stress to the brain. Each time such a stressor occurs, white matter in the brain dies off, resulting in rapid deterioration in motor function that is usually never regained. The disease varies in severity according to the genetic mutation involved, but it shortens life expectancy dramatically; most patients diagnosed survive just a few months to a few years after the first episode of regression.
The Nationwide Children’s research team worked with collaborators from the University of Utah to study astrocyte-targeted, AAV-packaged gene supplementation therapies in two mouse models of VWM. They gave mice from each model type multiple versions of AAV-delivered therapy as well: one that used a full-length astrocyte promoter — a piece of DNA that turns on gene expression in specific cells — which they expected to be too big to fit within the virus, and one that used a shortened version developed by another research group.
“The most challenging part about developing an astrocyte-targeted gene therapy was the small packaging capacity of AAV,” says Jessica Herstine, MS, a PhD candidate at The Ohio State University and researcher in the Bradbury Lab in the Center for Gene Therapy in The Abigail Wexner Research Institute at Nationwide Children’s. She is the lead author of the article detailing the research, which was selected as the cover story for June 2024 for Molecular Therapy and featured in a peer commentary for the same issue. “Since our gene of interest is large, we could only use small promoters to target astrocytes. That’s why our full-length AAV9-GFAP-EIF2B5 vector didn’t show much benefit.”
They have since developed an alternative version that they constructed based on the shortened version, to which they added back in sections of DNA they felt could be important. The novel astrocyte-specific promoter drives EIF2B5 expression and fits perfectly within AAV. The team is now testing their novel version in both mouse models used for the recently published study.
“I think we are quickly closing in on a lead gene therapy candidate,” says Allison Bradbury, PhD, principal investigator in the Center for Gene Therapy, who was instrumental in the development of two gene therapies now in clinical testing for Krabbe disease, a similar neurodegenerative white matter disorder. “Excitingly, we have many VWM mice living beyond a year of age from the truncated-promoter therapy described in the paper. We more recently injected additional mice with our novel promoter, so we need some time to see if it outperforms the truncated promoter construct.”
After a lead candidate for VWM is identified, several other preclinical tests need to be performed before it can move to human studies.
“We treated all of these mice neonatally, which is the best-case scenario, but there currently is not a newborn screening test for VWM, so it is most often not picked up until symptoms arise,” says Dr. Bradbury, who also has federal funding for studies into related diseases that may benefit from similar therapeutic approaches targeting astrocytes and other specific brain cell types, including tubulin folding cofactor D mutations and neurofibromatosis types 1 and 2. “After preclinical dose-ranging studies, which we already have underway with our top candidates, we will look at timing of the intervention to study the impact of therapy after symptom onset, then safety and tolerability studies in healthy animals.”
Even with such promising preclinical studies, human trials could be years away. But the findings give hope in a field that has struggled to find therapeutic options for many years.
“Having met patients and their families, I’ve seen firsthand how traumatic and devastating this disease is, especially since there isn’t an effective treatment,” says Herstine. “Although this is only the first step in developing a therapy for VWM, we hope our efforts help to expedite the process and emphasize the need for a life-saving treatment.”
Reference:
Herstine JA, Chang PK, Chornyy S, Stevenson TJ, Sunshine AC, Nokhrina K, Rediger J, Wentz J, Vetter TA, Scholl E, Holaway C, Pyne NK, Bratasz A, Yeoh S, Flanigan KM, Bonkowsky JL, Bradbury AM. Evaluation of safety and early efficacy of AAV gene therapy in mouse models of vanishing white matter disease. Mol Ther. 2024 Mar 27:S1525-0016(24)00212-0.
Image credit: Bradbury Lab at Nationwide Children’s Hospital
About the author
Katherine (Katie) Brind’Amour is a freelance medical and health science writer based in Pennsylvania. She has written about nearly every therapeutic area for patients, doctors and the general public. Dr. Brind’Amour specializes in health literacy and patient education. She completed her BS and MS degrees in Biology at Arizona State University and her PhD in Health Services Management and Policy at The Ohio State University. She is a Certified Health Education Specialist and is interested in health promotion via health programs and the communication of medical information.
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 28, 2014
- Post Tags:
- gene therapy
- Neurology