Transforming Medical Science Through Research Affinity Groups
Transforming Medical Science Through Research Affinity Groups https://pediatricsnationwide.org/wp-content/themes/corpus/images/empty/thumbnail.jpg 150 150 Katie Brind'Amour, PhD, MS, CHES Katie Brind'Amour, PhD, MS, CHES https://pediatricsnationwide.org/wp-content/uploads/2021/03/Katie-B-portrait.gifPurposeful synergy drives the most meaningful medical science. Nephrology physician-scientists require tissue samples, urologists desire tests to know which patients truly require surgery, and basic scientists must find ways to meaningfully assess new animal models to yield clinically valuable data.
If each of these professionals had a defined network of colleagues from the other disciplines — colleagues knowledgeable about their areas of interest and willing to collaborate — research and care could take a leap forward.
The scientist could study biomarkers to identify patients that most need surgery, the urologist could collect tissue samples on nephrology patients head – ed to the operating room, and nephrologists could teach bench scientists how to do a renal ultrasound on models to measure disease severity. Everyone would get what they need, and together, these experts would advance patient care and medical knowledge.
This interdisciplinary, communication-oriented approach to clinical and translational research is at the heart of the Nephrology and Urology Research Affinity Group (NURAG) at Nationwide Children’s Hospital. The group was founded by a developmental biologist and anatomist at Nationwide Children’s — Kirk McHugh, PhD, now director of the Division of Anatomy at The Ohio State University College of Medicine — eager to do something clinically useful with his newly discovered megabladder mouse model. The original participants loved the early gatherings so much that NURAG organically evolved (over 15 years of monthly meetings) into a broad group of dozens of physician-researchers and basic scientists with an interest in the overlapping areas of urology and nephrology.
The group meetings include a planned speaker, either from within NURAG membership or invited from another institution. The presenter shares in-progress research, a manuscript planned for publication, or a talk about a less scientific area of medicine that affects members as well, such as quality improvement or advocacy. The audience gets to learn about something relevant and new, and the speaker gets thoughtful, well-rounded feedback from experts in numerous disciplines. And the whole group benefits from new insights and knowledge in their field, plus an abundance of spirited discussion and ideas for future exploration.
Best of all, members say, the atmosphere is friendly and fosters intellectual exchange and collaboration among multiple disciplines, giving birth to relationships and research projects that may otherwise not have seen the light of day.
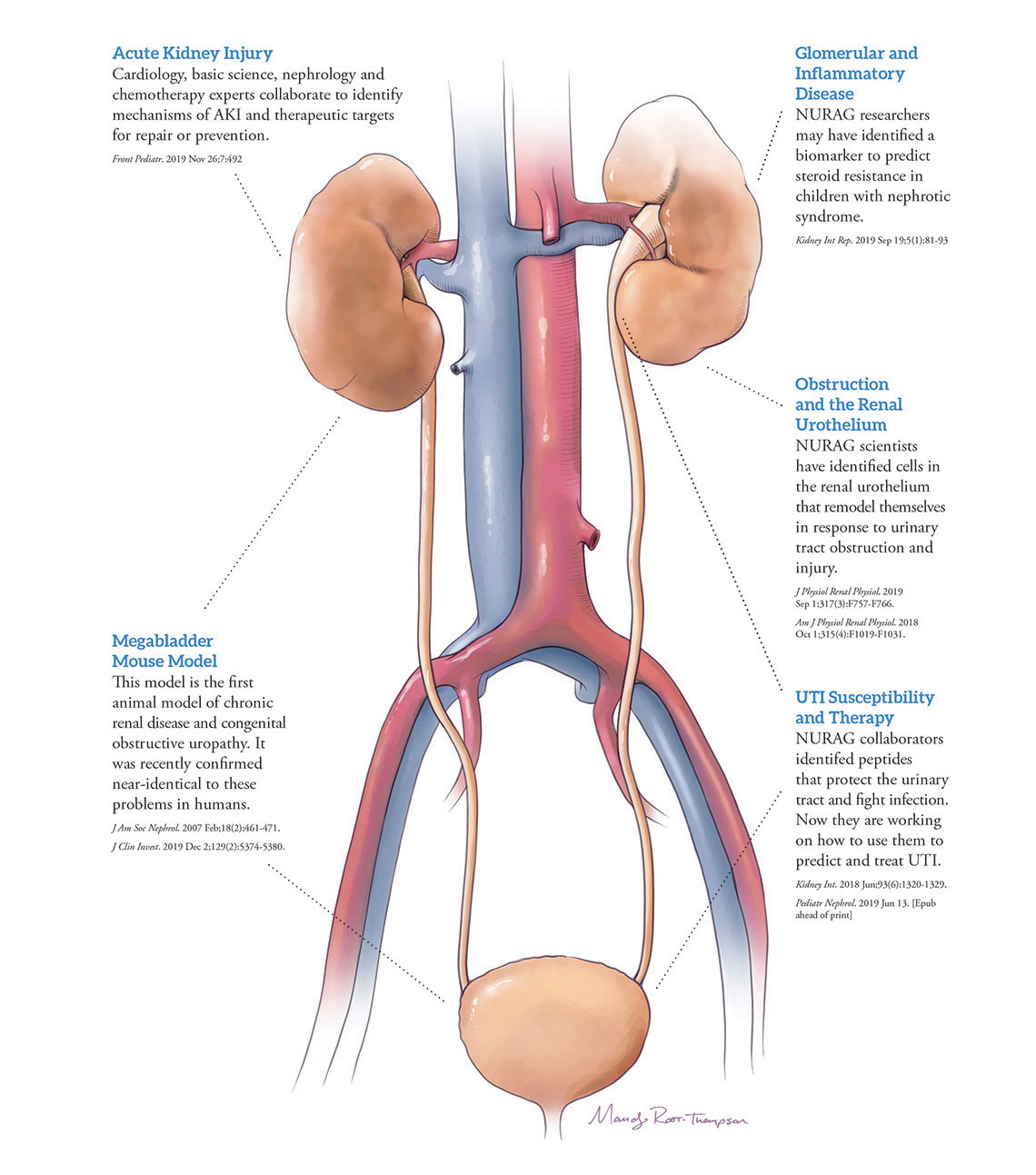
The Brainchildren of NURAG
Members of NURAG have built some of the country’s largest — and best-rated — pediatric research programs in both urology and nephrology, with research encompassing everything from mouse models to natural urinary tract infection (UTI) prevention. The collaborations involve more than just lip service to the concept of translational research, and often directly influence work done both by the group’s clinical members and bench scientists on a daily basis.
Megabladder Mouse: The Original NURAG Brainchild
When Dr. McHugh first pushed to establish NURAG, he did so to unite basic science researchers like himself with curious clinicians for the advancement of pediatric urology and nephrology care. His research at the time centered around the megabladder mouse model, which became the first animal model of congenital obstructive nephropathy and chronic kidney failure. He was eager for input from colleagues in urology and nephrology to help him plan better early studies for maximum translational impact for their patients. The partnership resulted in a co-led National Institutes of Health grant with NURAG co-founder Carl Bates, MD, now chief of the Division of Pediatric Nephrology at Children’s Hospital of Pittsburgh, to investigate the mutation’s clinical implications.
The studies of Dr. McHugh and his colleagues have illuminated much about the early development and disease progression of congenital obstructive nephropathy, one of the leading causes of chronic kidney failure in children. Most recently, he had the satisfaction of validating the model; collaborators in Europe identified several human families with genetic changes and disease sequelae that directly parallel those observed in the megabladder mouse.
This watershed model has played diverse roles in numerous scientific advancements in the field and has recently had a resurgence in interest due to potential applications in the study of urinary tract remodeling after injury — now a major area of focus for Dr. McHugh’s NURAG proteges and mentees.
Urinary Tract Obstruction and Injury
NURAG collaborators Brian Becknell, MD, PhD, a nephrologist at Nationwide Children’s and NURAG’s current director; Ashley Jackson, PhD, a postdoctoral fellow in the Center for Clinical and Translational Research in the Abigail Wexner Research Institute (AWRI) at Nationwide Children’s; Dr. McHugh and other clinician-scientists at Nationwide Children’s have long worked to understand the renal response to urinary tract obstruction in the megabladder mouse.
Their joint efforts have identified that the renal urothelium (tissue lining the drainage system of the kidneys) remodels itself to help protect the kidney during urinary tract obstruction. When obstruction occurs and urine is retained in the kidneys, these cells adapt to create a urine-proof barrier by forming a urothelial plaque, which allows expansion and provides structural support to the kidney, thus protecting it from damage. Dr. Jackson also recently identified the progenitor (cellular origin) of the protective urothelial cell.
“It’s compelling to think that if we can better understand the process by which progenitor cells form the protective cells, we can maybe drive intrarenal-urothelial remodeling to protect the kidneys from obstructive disease, starting in mice but ultimately translating our work to children,” says Dr. Jackson. The multidisciplinary team recently published their findings in the American Journal of Physiology-Renal Physiology.
UTI Pathogenesis and Treatment
Another key area of research for the clinicians and scientists in NURAG is urinary tract infection (UTI) — including who may be particularly susceptible and why — as well as what these findings mean for new treatment options. The efforts of John David Spencer, MD, chief of Nephrology at Nationwide Children’s, and his lab in the Center for Clinical and Translational Research in the AWRI have benefited greatly from NURAG-facilitated collaboration with the labs of Dr. Becknell; Christina Ching, MD, a urologist and clinician-researcher at Nationwide Children’s; and Sheryl Justice, PhD, a principal investigator in the Center for Microbial Pathogenesis in AWRI.
Dr. Spencer’s lab focuses on antimicrobial peptide (AMP)-related infection responses and related downstream effects, which dovetails with Dr. Justice’s expertise in the body’s natural formation of bacterial films, Dr. Ching’s work on innate immunity and host response to infection, and immunology and physiology work done by other basic science collaborators. Together, these research teams have explored the roles of AMPs and ribonuclease “superfamilies” in the urinary tract. Fluctuation of AMPs influences the body’s susceptibility to infection and its ability to fight infection-causing bacteria, such as E. coli, in the urethra, bladder, ureters and kidneys.
The group is rapidly making progress toward tracking and manipulating the production of AMPs and related molecules in the urinary tract to predict, prevent and even treat UTI in the near future.
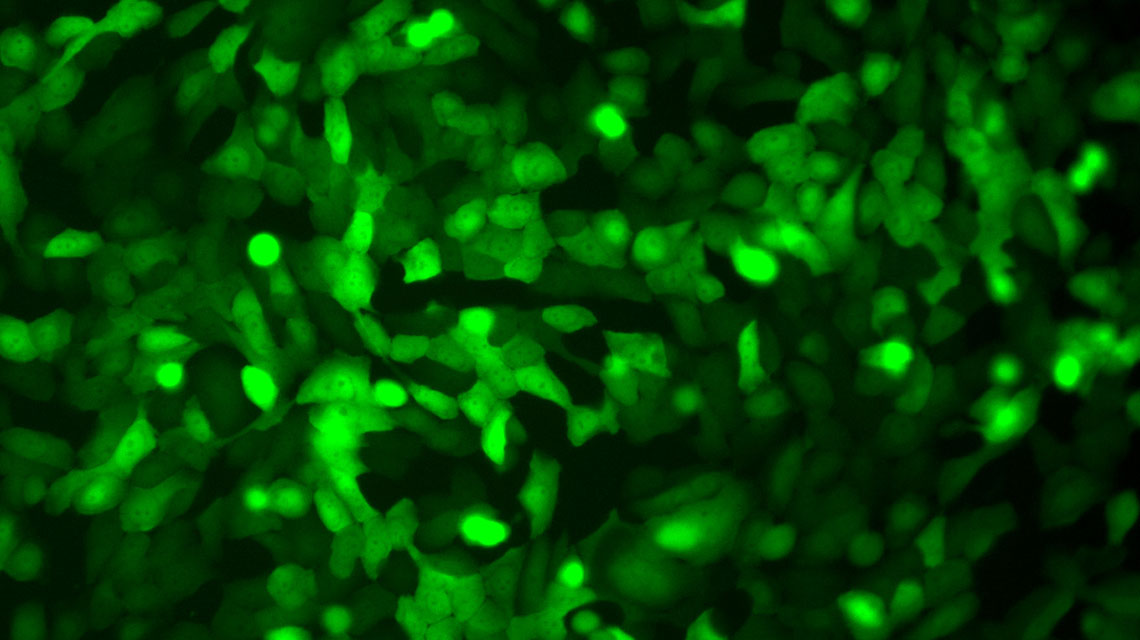
Antimicrobial peptides, identified by green immunofluorescent staining, are produced by human kidney cells. Fluctuations in AMPs influence the body’s susceptibility to infection.
Glomerular Diseases
Glomerular diseases and inflammatory diseases of the kidneys are another area of focus for NURAG participants. Shipra Agrawal, PhD, a principal investigator in the Center for Clinical and Translational Research, has a longstanding collaboration with nephrologist William Smoyer, MD, vice president and director for the Center for Clinical and Translational Research.
Together, they have studied molecular pathways involved in the function and injury of the kidneys’ glomerulus and podocytes, which filter toxins from the blood. By further extending their collaborations to include members of the Midwest Pediatric Nephrology Consortium, the team has recently identified potential biomarkers to predict steroid resistance in young nephrotic syndrome patients. The work appeared last fall in Kidney International Reports.
Mechanisms of Acute Kidney Injury
Another burgeoning area of focus for NURAG is championed by a cardiologist rather than a nephrologist or urologist. Catherine Krawczeski, MD, chief of the Division of Cardiology and co-director of The Heart Center at Nationwide Children’s, studies acute kidney injury following cardiopulmonary bypass. Now, NURAG’s acute kidney injury discussions are also expanding to include chemotherapy-induced injury and possible therapeutic targets for kidney disorders, thanks to recent additions to the group from The Ohio State University’s pharmacy program and a new physician-scientist on Nationwide Children’s nephrology team.
Future Plans and Opportunities for Growth
In addition to the key areas of research thriving under the umbrella of NURAG, collaborative opportunities continue to emerge. Unique synergies include that with Rachel Cianciolo, VMD, PhD, a veterinary pathologist in the Department of Veterinary Biosciences at The Ohio State University, and co-director of the International Veterinary Renal Pathology Service. After presenting her own work on kidney diseases in animals to NURAG members, Dr. Cianciolo began working with NURAG researchers at Nationwide Children’s to consult on the use of animal models for various kidney disorders and to score tissue samples for glomerular disease.
Veterinary colleagues such as Dr. Cianciolo are just the tip of the affinity iceberg. Chemists, neurologists, geneticists, bacteriologists, hematologists, biostatisticians, mathematicians, immunologists, cell biologists and more all play important roles in the advancement of clinical and translational investigations at Nationwide Children’s and beyond.
Self-Propagating Translational Research
Perhaps the greatest attribute of NURAG is its potential to encourage young clinicians and investigators to consider launching a new study or to specialize in urology or nephrology — while also supporting them in their research and training. This was certainly the case for several of its current members, including the group’s director.
“I grew up with NURAG, so to speak,” says Dr. Becknell, who first experienced the group as a medical student. “It’s one of the main reasons I chose to specialize in nephrology and stay here for my residency and fellowship. I liked to see surgeons, clinicians and medical students getting together in a nonintimidating environment to share ideas. I’ve benefitted hugely from the level of support it provides.”
He’s not the only one whose career trajectory was significantly influenced by participating in NURAG. Dr. Jackson started in Dr. McHugh’s lab during her doctoral studies and enjoyed the collaborative community so much that she chose to stay for her postdoctoral work. The training environment and mentorship provided by NURAG helped her secure a National Research Service Award Individual Postdoctoral Fellowship (F32), and she is pursuing additional NIH funding to become a principal investigator. She now serves as NURAG’s program coordinator and credits NURAG for launching her research career through early opportunities to grow and succeed, including mentorship of younger trainees.
This cultivation of the next generation of researchers is key to NURAG’s mission. The group regularly offers all participants the option to practice their presentations or submit their written work for review, ensuring that their research products are defensible, thorough and thoughtful. They also hire and provide travel funding for students, residents and fellows, and they are seeking NIH grants to begin supporting full NURAG trainee funding.
“Supporting each other and the next generation in the advancement of relevant, powerful research is the best legacy NURAG can leave,” says Dr. Ching, who credits her series of NIH grants to close relationships with her mentors, all of whom are NURAG members. “It truly is a breeding ground for new pediatric urology and nephrology clinicians and scientists.”
Building a Successful Research Affinity Group
The recipe for a successful research affinity group is probably flexible, but it is evident that it must include researchers both from the clinical world and basic science. It is also essential for participants to be curious, collegial and engaged.
Dr. Becknell believes it is the mix of new and experienced participants, as well as the relaxed but eager exchange of ideas of true scientific and clinical interest — rather than an emphasis on publication expediency or grant money competition — that creates the group’s unique appeal and, ultimately, its tremendous success.
“You feel such support knowing your colleagues are willing to help you advance your research,” Dr. Spencer agrees. “People are naturally attracted to it, and it impresses upon the next generation of physicians and scientists the value of doing collaborative work. Even those researchers who start off expecting to be independent quickly see the benefits of NURAG and fall into the fold.”
Former Nationwide Children’s clinicians have appreciated the NURAG community so much they have attempted to develop similar affinity groups at their new institutions. For others interested in doing the same, an affinity group obviously requires logistical support: space to meet, eventual financial support from grants or institutional research funds, and administrative support for the time required to meet and mentor each other.
As a group expands, so do the paperwork and planning needs. That’s why NURAG has worked to obtain institutional funding both for a biostatistician and a clinical research coordinator, who can facilitate the research done in the hospital’s Urology and Nephrology Combined Clinic and increase the support available to new investigators.
The snowball effect of knowledge generation and collaboration with the fields’ future leaders cannot be underestimated in its potential to change clinical care. Together, NURAG members publish numerous peer-reviewed papers each year — with well over 100 collaborative publications since its founding and numerous multidisciplinary, co-led NIH grants — and regularly present research at professional conferences.
NURAG participants believe this is just the beginning: new researchers join regularly, funding is growing, and subspecialty groups and collaborative grants will be priorities in 2020 and beyond.
The benefits of NURAG have been so apparent that Dennis Durbin, MD, MSCE, chief scientific officer at Nationwide Children’s, has encouraged and supported the emergence of three additional affinity groups across research and clinical staff: one to study the oral and gastrointestinal microbiome, one for neuroscience research, and one general pediatrics research affinity group. It is expected that additional groups may form as experts in other disciplines see their many benefits.
“If we can inspire young people, through an environment that supports curiosity, to consider a career in research that has something to do with the kidneys or urinary tract, that guarantees a positive future for our fields,” says Dr. Becknell. “But I think the fact that we all have a ton of fun is also a big part of what keeps this thing going.”
References:
- Ching CB, Gupta S, Li B, Cortado H, Mayne N, Jackson AR, McHugh KM, Becknell B. Interleukin-6/Stat3 signaling has an essential role in the host antimicrobial response to urinary tract infection. Kidney International. 2018 Jun;93(6):1320-1329.
- Ching C, Schwartz L, Spencer JD, Becknell B. Innate immunity and urinary tract infection. Pediatric Nephrology. 2019 Jun 13. [Epub ahead of print]
- Eichler T, Bender K, Murtha MJ, Schwartz L, Metheny J, Solden L, Jaggers RM, Bailey MT, Gupta S, Mosquera C, Ching C, La Perle K, Li B, Becknell B, Spencer JD. Ribonuclease 7 shields the kidney and bladder from invasive uropathogenic Escherichia coli infection. Journal of the American Society of Nephrology. 2019 Aug;30(8):1385-1397.
- Gooding JR, Agrawal S, McRitchie S, Acuff Z, Merchant ML, Klein JB, Smoyer WE, Sumner SJ; Midwest Pediatric Nephrology Consortium. Predicting and defining steroid resistance in pediatric nephrotic syndrome using plasma metabolomics. Kidney International Reports. 2019 Sep 19;5(1):81-93.
- Houweling AC, Beaman GM, Postma AV, Gainous TB, Lichtenbelt KD, Brancati F, Lopes FM, van der Made I, Polstra AM, Robinson ML, Wright KD, Ellingford JM, Jackson AR, Overwater E, Genesio R, Romano S, Camerota L, D’Angelo E, Meijers-Heijboer EJ, Christoffels VM, McHugh KM, Black BL, Newman WG, Woolf AS, Creemers EE. Loss-of-function variants in myocardin cause congenital megabladder in humans and mice. Journal of Clinical Investigation. 2019 Dec 2;129(12):5374–5380.
- Jackson AR, Hoff ML, Li B, Ching CB, McHugh KM, Becknell B. Krt5+ urothelial cells are developmental and tissue repair progenitors in the kidney. American Journal of Physiology: Renal Physiology. 2019 Sep 1;317(3):F757-F766. Jackson AR, Li B, Cohen SH, Ching CB, McHugh KM, Becknell B. The uroplakin plaque promotes renal structural integrity during congenital and acquired urinary tract obstruction. American Journal of Physiology: Renal Physiology. 2018 Oct 1;315(4):F1019-F1031.
- Nie X, Chanley MA, Pengal R, Thomas DB, Agrawal S, Smoyer WE. Pharmacological and genetic inhibition of downstream targets of p38 MAPK in experimental nephrotic syndrome. American Journal of Physiology: Renal Physiology. 2018 Apr 1;314(4):F602-F613.
- Singh S, Robinson M, Nahi F, Coley B, Robinson ML, Bates CM, Kornacker K, McHugh KM. Identification of a unique transgenic mouse line that develops megabladder, obstructive uropathy, and renal dysfunction. Journal of the American Society of Nephrology. 2007 Feb;18(2):461-71.
Image credits: Nationwide Children’s, artwork created for Nationwide Children’s by Mandy Root-Thompson
About the author
Katherine (Katie) Brind’Amour is a freelance medical and health science writer based in Pennsylvania. She has written about nearly every therapeutic area for patients, doctors and the general public. Dr. Brind’Amour specializes in health literacy and patient education. She completed her BS and MS degrees in Biology at Arizona State University and her PhD in Health Services Management and Policy at The Ohio State University. She is a Certified Health Education Specialist and is interested in health promotion via health programs and the communication of medical information.
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 28, 2014







