Sickle Cell Lung Disease: Opportunities to Advance Care and Research
Sickle Cell Lung Disease: Opportunities to Advance Care and Research https://pediatricsnationwide.org/wp-content/uploads/2021/03/AdobeStock_137900548-sickle-cell-header-1024x575.gif 1024 575 Pam Georgiana Pam Georgiana https://pediatricsnationwide.org/wp-content/uploads/2023/07/May-2023.jpg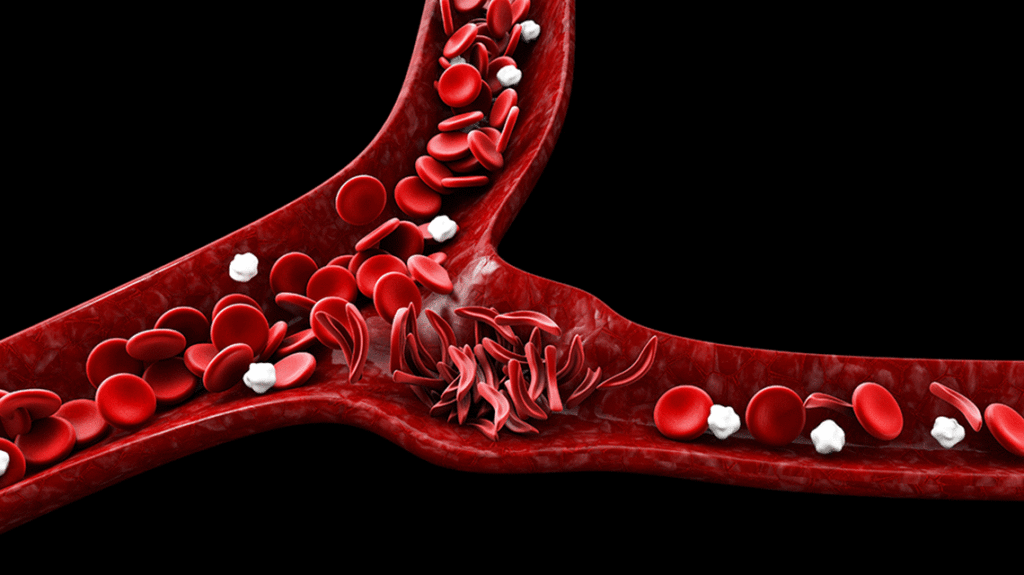
A series of studies aims to close gaps by integrating immunology, microbiology and environmental health into clinical research.
For children with sickle cell disease, lung complications remain among the most serious and least predictable drivers of morbidity and mortality. Despite advances in supportive care and disease-modifying therapies, clinicians still lack reliable tools to predict which patients will develop severe pulmonary complications such as acute chest syndrome, how acute events progress to chronic lung injury, or who will benefit most from targeted interventions. At Nationwide Children’s Hospital, a new series of studies aims to close those gaps by integrating immunology, microbiology and environmental health into longitudinal clinical studies.
That effort will be led by Benjamin Kopp, MD, MPH, ATSF, FAAP, who returned to Nationwide Children’s in March 2026 as chief of the Division of Pulmonary, Sleep Medicine and Cystic Fibrosis. Dr. Kopp completed his pediatric residency, fellowship training and early faculty work at Nationwide Children’s before spending four years at Emory University, where he expanded a nationally recognized research program in sickle cell and other lung diseases.
“Many of the questions we are asking now came from my time as a fellow and junior faculty member,” Dr. Kopp says. “What has changed is our ability to measure biology and environment together in ways that can directly inform care.”
From Clinic Observations to Longitudinal Science
In 2014, Dr. Kopp helped establish one of the nation’s early multidisciplinary sickle cell clinics at Nationwide Children’s, integrating pulmonology into routine sickle cell care. Outcomes from that clinic informed early pilot studies that formed the foundation of a multi-site longitudinal study that began at Emory and will continue at Nationwide Children’s in partnership with Emory and St. Jude Children’s Research Hospital.
The study follows children with sickle cell disease for at least five years and compares them with age- and race-matched siblings without the disease. During routine clinic visits and hospitalizations, investigators collect blood and airway samples, along with details clinical data. The team will deploy advanced bioinformatics and single-cell immune profiling to understand how immune pathways, microbes and environmental exposures interact over time.
“We do not have good predictors for complications like acute chest syndrome,” Dr. Kopp explains. “Treatment is largely reactive and often nonspecific. Most children receive antibiotics, even though many episodes may not be infectious.”
The “Exposome” Meets the Microbiome
A defining feature of the program is the use of a public health exposome framework, developed by environmental health researchers at The Ohio State University, including Darryl B. Hood, PhD. The exposome refers to the full range of environmental and social exposures a person experiences over time and how those exposures influence health. In this research, the goal is to understand how factors such as air quality, housing conditions and broader social environments shape immune responses and drive lung disease progression.
“The immune system does not operate in isolation,” Dr. Kopp says. “It is shaped by both microbes and by the environments children live in. Studying those interactions together allows us to identify modifiable factors and biomarkers that can guide prevention and treatment.”
Initial analyses focus on protein and metabolite signatures associated with acute chest syndrome and chronic lung injury. Environmental factors such as air pollution and microplastics are being examined in parallel, though these components remain in the early stages of investigation.
Supporting Life-Long Health
Michelle Gillespie, MD, focuses on the high-risk transition from pediatric to adult care for patients with sickle cell lung disease, building directly on the biologic insights generated through Dr. Kopp’s research. Dr. Gillespie’s work applies research findings to a critical clinical period when patients are at a heightened risk for worsening outcomes.
“Transition is a particularly vulnerable time,” Dr. Gillespie says. “Many patients who grow up with lung disease may not understand their disease. For example, they may become accustomed to symptoms like shortness of breath and not realize that it could signal serious complications.”
Unlike cystic fibrosis and many other chronic conditions, sickle cell disease lacks standardized transition guidelines and educational tools. Dr. Gillespie is beginning her research by assessing what patients and providers know, as well as identifying the specific information they want and need. Based on those findings, she plans to develop educational resources and clinical guidance for patients and providers as they move toward adult care.
Her research will incorporate biomarkers identified through Dr. Kopp’s longitudinal study to identify adolescents and young adults at higher risk for poor pulmonary outcomes and inform earlier, more targeted interventions.
Importance of Community Involvement
Both investigators emphasize that families and caregivers are essential partners in this work. Community input will help shape study design, recruitment and long-term sustainability, particularly in a field that has historically received limited research funding.
“There is still so much we do not understand” says Dr. Kopp. “But by committing to long-term, community-informed research, we can begin to close the gap between what we see in the clinic and what we can actually change for children living with chronic lung disease.”
Parallels Between Two Lung Diseases
Dr. Kopp’s research intentionally spans both sickle cell disease and cystic fibrosis, examining shared and distinct drivers of chronic lung injury. While cystic fibrosis has benefited from transformative therapies, chronic inflammation and limited global access remain significant challenges. In sickle cell disease, therapeutic options are far more constrained.
“In cystic fibrosis, the new therapies are now appropriate or available for every patients,” Dr. Kopp says. “In sickle cell disease, therapy options are even more limited. Studying these conditions side by side helps us identify pathways that may overlap and those that differ, which could lead to safer and more accessible therapies.”
His long-term goal is to advance personalized, immune-based treatment strategies that reduce hospitalizations, preserve lung function and extend life expectancy for patients with both conditions.
This article appeared in the 2026 Spring/Summer print issue. Download the issue here.
Image credits: Adobe Stock (header); Nationwide Children’s (portraits)
About the author
Pam Georgiana is a brand marketing professional and writer located in Bexley, Ohio. She believes that words bind us together as humans and that the best stories remind us of our humanity. She specialized in telling engaging stories for healthcare, B2B services, and nonprofits using classic storytelling techniques. Pam has earned an MBA in Marketing from Capital University in Columbus, Ohio.
- Pam Georgianahttps://pediatricsnationwide.org/author/pam-georgiana/
- Pam Georgianahttps://pediatricsnationwide.org/author/pam-georgiana/
- Pam Georgianahttps://pediatricsnationwide.org/author/pam-georgiana/
- Pam Georgianahttps://pediatricsnationwide.org/author/pam-georgiana/
- Posted In:
- In Sight
- Research
- Uncategorized