How Language-Processing Technology Could Transform Medical Practice, Research and Patient Participation
How Language-Processing Technology Could Transform Medical Practice, Research and Patient Participation https://pediatricsnationwide.org/wp-content/themes/corpus/images/empty/thumbnail.jpg 150 150 Katie Brind'Amour, PhD, MS, CHES Katie Brind'Amour, PhD, MS, CHES https://pediatricsnationwide.org/wp-content/uploads/2021/03/Katie-B-portrait.gifRecent revolutions in researchers’ ability to process natural language sources, such as clinic visit notes, transcripts or medical diaries, could dramatically expand opportunities to improve health care and prevention health outreach.
Natural Language Processing (NLP) is a subfield of computer science and artificial intelligence that deals with the interaction between computers and human language. It uses algorithms and computational techniques to analyze and understand human language in both written and spoken forms (such as, speech, transcripts, written notes, social media posts, publications, etc.). NLP applications have been gradually evolving for many years and have recently reached a level of sophistication that may greatly improve their utility in the field of health care. According to researchers at Nationwide Children’s Hospital, who have already incorporated numerous NLP-based applications into clinical and investigative work, the potential benefit of these technologies could be groundbreaking for physicians and patients alike.
“Technological advancements in health care, particularly in the field of natural language processing, have the potential to revolutionize the way physicians and patients interact, paving the way for a more personalized, efficient and effective health care experience,” says Emre Sezgin, PhD, principal investigator in the Center for Biobehavioral Health in the Abigail Wexner Research Institute at Nationwide Children’s. “NLP has the potential to unlock a wealth of insights hidden within the vast amounts of unstructured healthcare data, leading to better clinical decision-making, early disease detection and personalized treatment plans.”
As a 2022-2023 Challenge award winner from the Health Resources and Services Administration, Dr. Sezgin’s team has been working diligently to test and deploy conversational artificial intelligence (AI) applications for social needs identified proactively by patients or by clinicians during visits.
The project relies on a technology known as a chatbot (named Daphne©), which uses an AI-based conversation tool to communicate with natural language (speech or text) and intelligently provide highly relevant, service-oriented resources for patients and families.
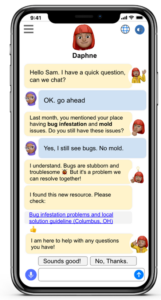 “Daphne is iteratively designed by our team in the light of multidisciplinary stakeholders’ feedback, including primary care clinicians, nurses, social workers, researchers, family advocates and community health workers. It does social needs screening and shares personalized resources based on family needs. It also guides families on how to access the resources,” Dr. Sezgin says. “
“Daphne is iteratively designed by our team in the light of multidisciplinary stakeholders’ feedback, including primary care clinicians, nurses, social workers, researchers, family advocates and community health workers. It does social needs screening and shares personalized resources based on family needs. It also guides families on how to access the resources,” Dr. Sezgin says. “
“In the future, health care providers can gain a more complete understanding of a patient’s needs, preferences and social determinants of health by utilizing insights from chatbots like Daphne,” says Dr. Sezgin, who has authored many NLP- and AI-based research studies and perspectives.
Dr. Sezgin also envisions a future where “Daphne could also be a supplementary tool for social workers or community health workers, to ease the process of screening and providing timely feedback to support families.
Clinical Research Support
Nationwide Children’s investigators already used NLP to develop a clinical research support tool, DeepSuggest — an AI-driven assistant to support EMR search and suggestions. The project, which received Patient-Centered Outcomes Research Institute (PCORI) funding in 2018, has made great strides beyond prior similar technology. In a recent study, the program doubled the retrieval of clinically relevant notes in medical records compared with Epic when prompted with search terms, primarily by generating queries and offering suggestions to improve keyword searches. It does this through exploration of commonly related terms, spelling variations (even errors), abbreviations and acronyms, regardless of whether they are part of the system’s pre-existing nomenclature programs. A human can then review and make adjustments to the resulting list that DeepSuggest will use to probe the database of notes. The result is an EMR system add-on that can identify a greater quantity of relevant information in a patient cohort, which has obvious implications when examining a patient’s medical history or conducting retrospective reviews.
“DeepSuggest helped us to expand our research with more focus on rare disease patients and underrepresented populations,” notes Dr. Sezgin, part of the DeepSuggest project team, “allowing us to gain more knowledge about these populations derived from EMR and craft more effective policies and interventions to improve services and health outcomes.”
Envisioning the future of NLP in health care
As a new addition to the NLP and conversational AI domain, a more sophisticated form of machine learning, called generative AI, has recently been introduced. This level of technology produces content and mimics human linguistic capabilities (leveraging Large Language Models or LLM) with little to no training data — a major departure from traditional AI and ML applications, which typically require many thousands of example data points before producing valuable output. GPT has been the most popular example with the introduction of ChatGPT, and there are a growing number of studies examining its comprehension and the level of support it could offer in clinical practice.
Nationwide Children’s-based teams, including Dr. Sezgin’s, are studying applications of these models, such as GPT-3 and GPT-4, with the goal of building useful applications for the medical world and investigating how to operationalize such tools in compliance with rules and regulations (e.g., the Health Insurance Portability and Accountability Act) and other ethical standards. According to their research to date, a promising starting point may include patient triaging and clinical conversation summarization. However, there are number of crucial considerations for implementation and operations that must be better studied before it makes sense to deploy the technology in real-world medical settings.
“In the near future, current AI and ML applications, LLM and generative AI have potential to move health care to the next stage by supporting human- or team-AI collaborations, boosting innovation and productivity that complements and enhances clinicians’ expertise, and crafting new possibilities for patient care,” says Dr. Sezgin, who has also applied GPT models to support clinical charting for dental medical notes. “I am optimistic that such intelligent systems and human expertise will converge to create unprecedented advancements in diagnosis, treatment and patient well-being.”
References and Resources:
- Sezgin E, Sirrianni J, Linwood SL. Operationalizing and implementing pretrained, large artificial intelligence linguistic models in the US health care system: Outlook of Generative Pretrained Transformer 3 (GPT-3) as a service model. JMIR Medical Informatics 2022;10(2):e32875.
- Sezgin E, D’Arcy S. Editorial: Voice technology and conversational agents in health care delivery. Frontiers in Public Health 2022;10:887492.
- Sirrianni J, Sezgin E, Claman D, Linwood SL. Medical text prediction and suggestion using generative pretrained transformer models with dental medical notes. Methods Inf Med. 2022 Dec;61(5-06):195-200. doi: 10.1055/a-1900-7351. Epub 2022 Jul 14. PMID: 35835447..
- Moosavinasab S, Sezgin E, Sun H, Hoffman J, Huang Y, Lin S. DeepSuggest: Using neural networks to suggest related keywords for a comprehensive search of clinical notes. ACI Open 2021;05(01):e1-e12.
- Sezgin E, Hussain SA, Rust S, Huang Y. Extracting medical information from free-text and unstructured patient-generated health data using natural language processing methods: Feasibility study with real-world data. JMIR Form Res 2023;7;e43014.
- Boch S, Sezgin E. Ethical artificial intelligence in paediatrics. Lancet Child & Adolescent Health 2022;6(12):833-835.
- Hussain SA, Sezgin E, Krivchenia K, Luna J, Rust S, Huang Y. A natural language processing pipeline to synthesize patient-generated notes toward improving remote care and chronic disease management: a cystic fibrosis case study. JAMIA Open 2021;4(3):ooab084.
Image credit: Nationwide Children’s, courtesy of Emre Sezgin
About the author
Katherine (Katie) Brind’Amour is a freelance medical and health science writer based in Pennsylvania. She has written about nearly every therapeutic area for patients, doctors and the general public. Dr. Brind’Amour specializes in health literacy and patient education. She completed her BS and MS degrees in Biology at Arizona State University and her PhD in Health Services Management and Policy at The Ohio State University. She is a Certified Health Education Specialist and is interested in health promotion via health programs and the communication of medical information.
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 28, 2014






