The New Emergency Department — for Behavioral Health
The New Emergency Department — for Behavioral Health https://pediatricsnationwide.org/wp-content/uploads/2020/10/AdobeStock_86027188_header-1024x575.jpg 1024 575 Katie Brind'Amour, PhD, MS, CHES Katie Brind'Amour, PhD, MS, CHES https://pediatricsnationwide.org/wp-content/uploads/2021/03/Katie-B-portrait.gif
How pediatric hospitals are creatively tackling the unique care needs of a growing population of youths in crisis.
From attention deficit disorder to anxiety or depression, mental health conditions affect about 1 in every 5 children. While some of these cases resolve, many children go on to adulthood with mental or behavioral health disorders, and continue to suffer problems at home, school, work and in their social lives.
To make matters worse, numerous conditions — and their sequelae — are on the rise. According to the Centers for Disease Control and Prevention, incidence of depression and anxiety is growing among children ages 6-17. After accidents, suicide is the leading cause of death among kids 10 and older.
And of course, as in any health-related emergency, many families turn to the emergency department for care. From 2011 to 2015, more than 13 million youth (ages 6-24) presented to the ED with a psychiatric concern, according to a 2019 publication in Pediatrics. Unfortunately, more than half remained at the ED for 3 hours or more, and the vast majority (84%) were discharged without seeing any mental health professional.
A 2020 study in Pediatrics from Rachel Stanley, MD, division chief for Emergency Medicine at Nationwide Children’s Hospital, showed that in the period from 2007 to 2016, pediatric ED visits for deliberate self harm rose 329% and visits for all mental health disorders rose 60%.
The Problem With A Standard ED
While emergency departments should always be an option to treat young people in crisis (especially those in true medical emergency situations), they’re not often the best care solution. The vast majority of young people coming into EDs in a behavioral health crisis do not need medical care— they haven’t physically injured themselves and do not require clinical care for coexisting health conditions. Furthermore, more than 80% do not require hospital admission or transfer to an inpatient psychiatric facility.
Regardless, patients and their families sit in hectic rooms that are often ill-equipped for people in a mental health crisis. Surrounded by equipment with wires and cords, medication closets, and furniture with sterile design and purely medical purposes, problems such as anxiety, disorientation, suicidal ideation and violent behavior can easily amplify.
“What we learned from being in a traditional ED is that the environment just isn’t conducive to positive outcomes — we were assessing kids in gowns on hospital beds, and it didn’t feel good for our population,” says Ericka Bruns, LPCC-S, director of Acute Services at Nationwide Children’s Hospital. Prior to the opening of a range of new programs and facilities, her therapist team felt there was a better model of care they could achieve. “We wanted our new psychiatric crisis department consultation rooms to look very much like the outpatient setting — chairs and desks, warm colors and wide hallways, motor skill and comfort rooms, and spaces for kids with behavioral dysregulation to avoid restraint whenever possible. Through triage, we are able to find the right space in our environment that best suits their needs.”
As psychiatric visits to the ED grow (national visits for suicide-related incidents alone jumped 2.5-fold from 2011 to 2015), hospitals are struggling to accommodate the patient load from a staffing and a facility perspective. Patients with potential for suicide must be constantly supervised. Staff are frequently injured due to lack of training in psychiatric crisis management and the fact that the care environment is often oriented for medical rather than mental health care.
When mental health professionals are available, they are often not affiliated strictly with the ED and must be called in for consultation, resulting in lengthy waits. In the meantime, medical evaluations and lab tests further increase agitation, time and costs for families. And unfortunately, these tests are often uninfluential in clinical decision-making for these kids except in a small subset of cases — identifiable by history or an exam — according to the Health Resources and Services Administration’s toolkit for improving pediatric mental health care in the ED.
Unique Care Solutions
Recognizing the unsuitable and resource-draining nature of standard ED environments for children experiencing behavioral health concerns, many hospitals have sought out alternative ways to meet the needs of patients in crisis both through their facility and the type of care they provide.
These tactics are not quick, easy or (when they require new or renovated facilities) cheap. However, they can improve the quality and environment of care, reduce ED staff burden, improve parental satisfaction, reduce time to discharge, lower the cost of care, and decrease risks to patients and staff. Psychologically, they can also be much more calming for patients in fragile mental states.
Approaches include specialized ED rooms, integrated ED care teams, psychiatric EDs, teleheath crisis consultations, inpatient and partial hospitalization, bridge programs, hotlines and outpatient services.
Special ED Rooms
Perhaps the most straightforward facility accommodation hospitals can make is to triage visitors with a psychiatric concern to a separate waiting area — a room or hallway set up to be less stimulating and more like a living room. These provide calm, comfortable places to wait before or between services.
One step beyond separate waiting areas are special ED rooms designed to meet the needs of psychiatric patients while also fulfilling legal requirements for medical equipment and supplies. Ligatures and physical hazards can be locked away inconspicuously and accessed only as needed (for example, in hidden panels or behind cabinets or doors). The rooms can be painted or decorated to reduce the emphasis on medical treatment and instead promote more conversational care approaches.
Prior to the construction of its Psychiatric Crisis Department, Nationwide Children’s used this type of set-up, with five specialty behavioral health rooms set aside in the ED, a special bathroom safe for suicidal patients, and an integrated staffing model.
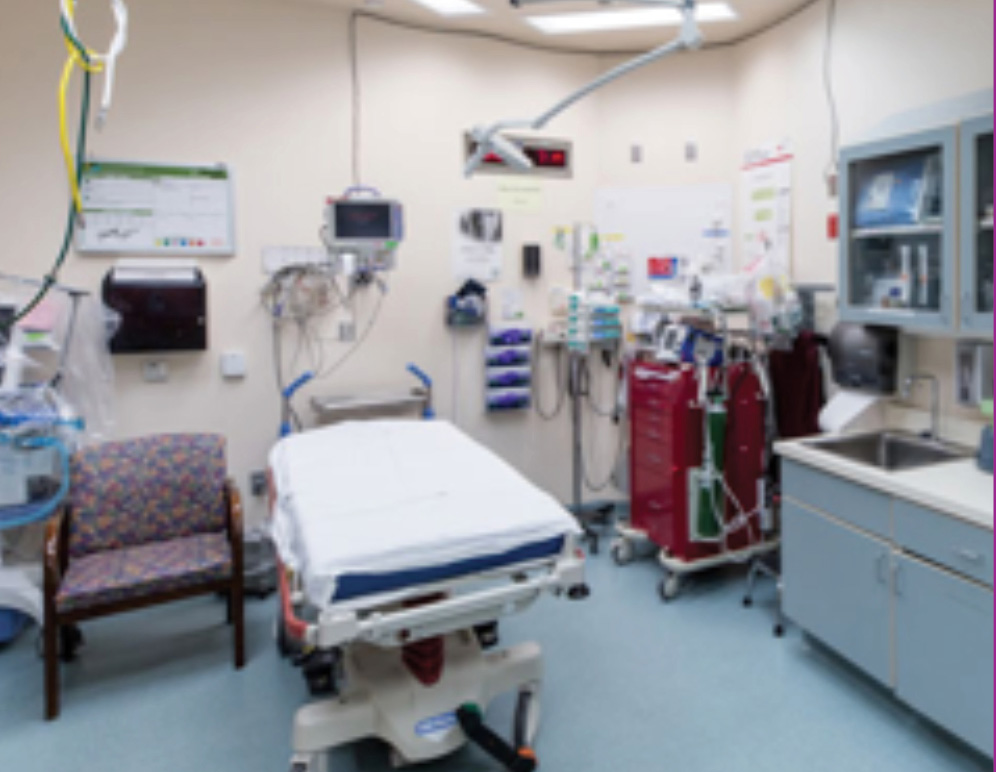
Figure 1. A standard Type A ED room requires medical beds, equipment, technology and medications to be easily accessible and available so that a minimum level of clinical care can be administered in any room. Staffing must also include 24-hour medical personnel. Although additional waiting rooms and customized care rooms or on-call/on-site psychiatry staff can also be present, the rooms and staff must still meet primary Type A ED requirements.

Figure 2. This Type B ED room at Dayton Children’s offers an environment like a living room or outpatient care room, set up to relieve anxiety, encourage conversation, avoid self-harm risks and minimize the “hospital” feel of the care spaces. Staffing balance can also emphasize the appropriate type of expertise. Care must still be available and provided to any comer at any time of day, but many set-up and staffing requirements are far more flexible than Type A EDs.
Integrated ED Care Teams
When feasible, hospitals can also address the behavioral health needs of ED patients through staffing. By committing a counselor, behavioral health social worker, nurse or pediatric psychiatrist to be on call or onsite, some of the burden can be removed from medical staff and transitioned to more appropriate providers.
On-call mental health professionals or staffers permanently based in the ED can provide suitable assessments and referrals and ensure patients receive adequate follow up after their visit.
While this collaboration is ideal for patients, it demands flexibility for co-locating staff, calling in providers from elsewhere in the hospital in short order, booting up telehealth services for remote consultations, or a solid understanding of demand — both throughout the day and seasonally — to adequately address patient needs without overstaffing the ED with mental health professionals.
If integrated staffing is not an option, ED staff can benefit from crisis stabilization and de-escalation training such as the Marcus Crisis Prevention Program offered by the Children’s Hospital of Atlanta, which helps reduce ED staff injuries and the need to use patient restraints. Their team has already trained more than 5,000 medical professionals around the world to offer more patient-friendly, risk-reducing care to psychiatric patients presenting at a standard ED, as well as to patients in other hospital departments.
Type B EDs or Psychiatric EDs
One unique approach, as taken by Dayton Children’s Hospital, involves reclassifying the type of center used for behavioral health emergencies. Rather than having patients in an emotional or psychiatric crisis treated in the standard (Type A) ED, patients can be triaged over the phone, through local care sites, or upon presentation (via self-selection if they follow signage) and sent directly to their Behavioral Crisis Center.
Their facility is able to avoid many of the staffing and equipment requirements for standard EDs by falling under the category of Type B emergency centers, per the Emergency Medical Treatment and Active Labor Act (EMTALA). This puts it more on par with labor and delivery departments, allowing it to customize the equipment, look and feel of the rooms—as well as the staffing—to the primary needs of its patients.
“Prior to opening the Behavioral Crisis Center, the volume of patients coming for strict behavioral health intervention and crisis in the ED was so strong that it was hard to keep up with the staffing and resources we had,” says Mindy Schultz, MSW, LISW-S, director for Social Care Services at Dayton Children’s. “We knew we needed to do more and have a dedicated service for kids in crisis, to expand our holistic continuum of care and fill those gaps in the system.”
The new set-up saves families about $1,000 per visit and more than an hour of ED visit time, compared to what patients averaged in the standard ED for less targeted treatment in the past.
In psychiatric-specific EDs, instead of wire-filled, medically oriented rooms, patients find chairs or a couch and desk in their room. Much as they would in an outpatient visit, they speak to staff conversationally, rather than wearing a medical gown and sitting on a hospital bed. Medical personnel are available for assessments as needed but make up the minority of care providers on staff, reversing the typical expertise balance compared to integrated Type A EDs.
Nationwide Children’s and the University of Pittsburgh Medical Center (UPMC) have similarly tailored ED solutions. The Psychiatric Crisis Department in Columbus and UPMC’s Psychiatric ED both have separate buildings focused exclusively on psychiatric care, with medical assistance available as needed and environments set up to be reassuring, safe and calming. While Nationwide Children’s is obviously focused exclusively on kids, UPMC has built in a pediatric specific section for their ED, which also has adult and acute milieus. Both approaches enable people in crisis or psychiatric emergencies to be evaluated, treated and
referred or admitted, if necessary, in more patient friendly environments than a standard medical ED.
Telehealth Crisis Consultations
In areas where access to pediatric mental health specialists is limited—or when it is infeasible to provide integrated care due to staffing or resource limitations — telehealth can expand the crisis services available in EDs, acute care settings or community centers. Remote consultations offer a novel way to improve access for crisis care when an ED is too remote, small or understaffed to have a psychologist or mental health social worker present at all times.
As virtual ED visits become more widely available and utilized, many mental health professionals are optimistic they will improve the quality of mental health care delivered to children presenting to standard EDs and result in better referrals and fewer readmissions.
To function most effectively, however, telehealth providers must be properly connected to community support services and aware of available care options for follow-up and referrals, to ensure kids end up with the ongoing care they require.
Nathan Call, PhD, clinical director and psychologist at the Marcus Autism Center at Children’s Hospital of Atlanta, revealed the effectiveness of telehealth for clinic-to-home parent coaching for patients with autism as part of a National Institutes of Health grant. When COVID-19 hit, the hospital ramped up and expanded their telehealth approach into other behavioral health services to reserve on-site visits for patients with only the most severe concerns. They, like Nationwide Children’s, are at least temporarily conducting virtually all nonurgent care via telehealth services.
“We’ve started to see real traction, and as more clinicians use telehealth, I believe it will increasingly become an accepted practice,” says Dr. Call. “Even after COVID, it will be hard to go back to everything — even emergency care — having to be in a brick and mortar establishment, especially since so many interventions have to involve the home environment anyway.”
Acute Inpatient Care and Partial Hospitalization
Inpatient care, offered through psychiatric departments using specialized inpatient beds and intensive assessments, surrounds patients with the expertise they require to get back on track. Acute care programs offer an alternative to typical inpatient admission, and often accept patients for a few days to a couple of weeks. Both of these program options are designed to offer intensive medical attention (including medication management), constant supervision and an evolving care plan designed to transition them to residential or partial hospitalization services — or, ideally, back home.
However, many hospitals suffer from a consistent shortage of beds for this type of care. To address this problem, some institutions have invested in specialized units and larger facilities to accommodate full-time inpatients, short-term “acute” care and day patients requiring less intensive care or supervision.
Nationwide Children’s, for example, built the new Big Lots Behavioral Health Pavilion, which opened in early 2020 and focuses primarily on acute services. After triage in its Psychiatric Crisis Center (a specialized
psychiatric ED), patients who need further assessment or intensive care step up to inpatient, partial hospitalization or a short-term intensive treatment stay in the Youth Crisis Stabilization Unit.
The Youth Crisis Stabilization Unit typically has about a three-day length of stay prior to transitioning patients into their ongoing treatment plan and is a step beyond short-term “non-admission” stays offered at some EDs (called the Extended Observation Suite at Nationwide Children’s), which give staff a day or so to assess patients and develop appropriate safety plans for transition in one direction or another. The three-day program has already demonstrated lasting reductions in suicidal ideation, improved functioning, increased readiness for transition and high levels of patient satisfaction 3 months after care.
Bridge Programs and Hotlines
“If you’re not in the mental health field, it’s like navigating a foreign country,” says Linda Richey, LISW-S, director of the Psychiatric Intake Response Center (PIRC) at Cincinnati Children’s Hospital Medical Center. The PIRC serves as a transitional and triage program to help direct patients to the proper level of initial care. “The bridge allows us to walk with the family through that, to navigate the system along with them to get that first appointment and make sure things are okay.”
Rather than even entering the ED, patients are initially triaged on the phone to determine if they meet criteria to be seen in an alternate location and receive the same
psychiatric assessment they would receive if they presented to the ED but in a more appropriate environment. In 2019 alone, the PIRC diverted 500 would-be ED patients to more appropriate venues for care.
Many other hospital systems, including Nationwide Children’s and UPMC, also have bridge programs (called the Critical Assessment and Treatment Clinic at Nationwide Children’s). Oftentimes, the programs function as hyperspecialized resource centers staffed by masters-level counselors, social workers and referral coordinators who are extremely familiar with local providers, programs and the resources available to help families obtain appropriate care after discharge from inpatient services or the ED. When the required services are not available without a waiting period, bridge programs also provide interim services until children can transition.
Crisis response programs, such as the Acute Crisis Response Team at Nationwide Children’s, may staff local hotlines and supplement ED triage needs, directing crisis callers to the most appropriate services, providing advice to parents and dispatching mobile response teams when needed.
When patients call into the UPMC PsychCare+ line, for example, the center serves as both a triage service and crisis hotline. Callers can receive some advice over the phone, get a referral or recommendation on where to seek care, or have a mobile response team or clinician sent to the home, school or other location to help with urgent on-location care. These teams often assess for suicide and make immediate safety or stabilization plans and referrals, as well as provide some coping education for patients and their families.
Outpatient Services and Community Embeddedness
Beyond their campus services, many children’s hospitals have also begun widespread behavioral health outreach initiatives. By boosting the community’s ability to recognize and respond to behavioral health concerns, and by training primary care providers in standardized suicide screening and basic intervention techniques, many local providers can help kids get into the right care at the right time.
Partners For Kids® — an accountable care organization operated in partnership with Nationwide Children’s — offers formal Project ECHO training in behavioral health to primary care providers, attempting to increase the chance kids will receive appropriate care without having to travel. The hospital also staffs mental health professionals in schools, satellite Primary Care Centers and Close to Home SM Centers, and is now researching the best approaches to telehealth consultation for distant EDs in order to offer more accessible psychiatric care regionally.
“Our community work is intentionally designed to support local providers and agencies to address more mental health conditions at less intensive levels, rather than refer to us,” says David Axelson, MD, chief of the Department of Psychiatry and Big Lots Behavioral Health Services at Nationwide Children’s. “We’re also hoping that our comprehensive community approach will reduce ED use for crisis patients, reduce readmissions and create a better pattern of service utilization, where outpatient and other interventions are successful enough to keep kids out of crisis care.”
Stigma Reduction and Crisis Prevention
While the rising incidence of suicide-related ED visits and behavioral health conditions is certainly cause for concern, some practitioners choose to consider optimistic explanations as part of the increase, citing a
reduction in stigma and improved awareness of mental health as a legitimate, treatable issue. Concerted efforts at stigma reduction are, in fact, a large part of some hospitals’ approach to improving care — by getting kids any care at all.
“A lot of kids experiencing symptoms aren’t receiving treatment, and that’s what our new building is about,” says Bruns. “It’s nine stories, smack downtown and all lit up. We want folks to know we’re not embarrassed to focus on behavioral health. It’s part of the whole child and it’s something to highlight.”
Coupled with the Caring Contacts crisis prevention text message service, Nationwide Children’s is targeting Zero Suicide, which involves universal screening for suicidal ideology — a tactic adopted in the hospital’s
extended care network at Cincinnati Children’s and numerous other pediatric institutions. In-hospital crisis response teams and staff training have further enabled progress toward reduced self-harm and improved patient experiences.
“We’ve been working hard to reframe the way we approach psychiatric care, flipping it on its head so that it is painstakingly patient-focused rather than clinician-focused,” says Elizabeth Sysak, MD, director of PsychCare+ and senior administrator over psychiatric emergency services at UPMC. Her program redesigned their psychiatric ED so that staff are fully visible and can see patients in each of their three segmented waiting areas at all times — a tactic that reduced safety incidents by half. Their off-site crisis center also works hard to avoid the typical “hospital vibe.”
Similar approaches to the patient experience at any level of behavioral health care can help maintain stability in the care environment. As hospitals incorporate patient-oriented approaches to design and décor, staff visibility and other resource set-ups (such as peer navigators and iPads), the entire experience shifts from one that induces anxiety to one that suits patient needs and helps prevent crisis escalation.
What’s Next for Pediatric Behavioral Health Crisis Care?
As stigma falls and growing numbers of hospitals expand or improve their approaches to serving kids in crisis, providers are hopeful for the future of behavioral health care. Locations with significant staff and financial resources aim to expand outreach via telehealth and mobile units, and specialized centers will now have the bandwidth to conduct better research on best practices and outcomes.
“The issue of getting people the care they need, when and how they need it, hasn’t been solved yet,” says Luke Kalb, PhD, assistant professor at the Kennedy Krieger Institute and lead author of a Pediatrics paper that helped draw attention to the nationwide increase in ED use for psychiatric problems. “There are no easy answers to this challenge. It’s going to require a lot of people to come to the table — providers, policymakers, insurers, hospital administrators and more — to really make concerted efforts and come up with effective long-term strategies.”
In the meantime, research emerging from specially designed facilities should help identify best practices and reveal which tactics are most effective in addressing community needs. By sharing the wide range of approaches and future outcomes from such programs, it is the hope of hospitals leading the way in behavioral health crisis care that all pediatric treatment programs will be able to adopt the most effective strategies in time.
This article appeared in the Fall/Winter 2020 print issue. Download the print now.
References:
- Lo CB, Bridge JA, Shi J, Ludwig L, Stanley RM. Children’s mental health emergency department visits: 2007-2016. Pediatrics. 2020;145(6):e20191536.
- National Alliance on Mental Illness. Mental health facts: Children & teens. No date.
- Centers for Disease Control and Prevention. Children’s mental health: Data and statistics on children’s mental health. 15 June 2020.
- National Institute of Mental Health. Suicide. April 2019.
- Kalb LG, Stapp EK, Ballard ED, Holingue C, Keefer A, Riley A. Trends in psychiatric emergency department visits among youth and young adults in the U.S. Pediatrics. 2019 April;143(4):e20182192.
- U.S. Department of Health and Human Services, Health Resources and Services Administration, Maternal and Child Health Bureau. Critical crossroads pediatric mental health care in the emergency department: A care pathway resource toolkit. Rockville, Maryland: U.S. Department of Health and Human Services. 2019.
- Ramtekkar U, Bridge J, Thomas G, Butter E, Reese J, Logan E, Lin S, Axelson D. Pediatric telebehavioral health: A transformational shift in care delivery in the era of COVID-19. JMIR Mental Health. 2020 Sep 18;7(9):e20157
- Lerman DC, O’Brien MJ, Neely L, Call NA, Tsami L, Schieltz KM, Berg WK, Graber J, Huang P, Kopelman T, Cooper-Brown LJ. Remote coaching of caregivers via telehealth: Challenges and potential solutions. Journal of Behavioral Education. 2020 Jun;29(2):195-221.
- McBee‐Strayer SM, Thomas GV, Bruns EM, Heck KM, Alexy ER, Bridge JA. Innovations in Practice: Intensive crisis intervention for adolescent suicidal ideation and behavior – an open trial. Child and Adolescent Mental Health. 2019 July 1;24(SS-8).
Image credits: Adobe Stock; Nationwide Children’s
About the author
Katherine (Katie) Brind’Amour is a freelance medical and health science writer based in Pennsylvania. She has written about nearly every therapeutic area for patients, doctors and the general public. Dr. Brind’Amour specializes in health literacy and patient education. She completed her BS and MS degrees in Biology at Arizona State University and her PhD in Health Services Management and Policy at The Ohio State University. She is a Certified Health Education Specialist and is interested in health promotion via health programs and the communication of medical information.
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
- Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 28, 2014
- Posted In:
- Features







