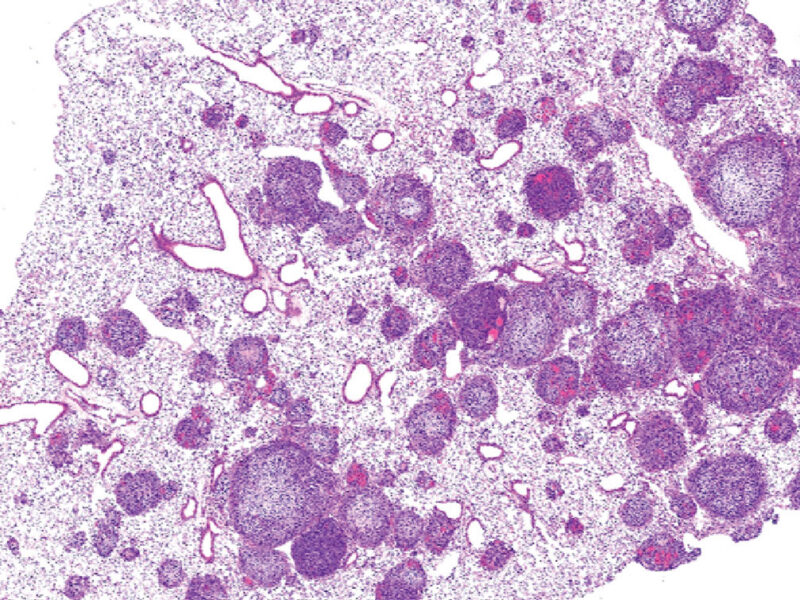
For AYA Females With Rhabdomyosarcoma, Consider Routine Examination or Imaging of Breasts
For AYA Females With Rhabdomyosarcoma, Consider Routine Examination or Imaging of Breasts https://pediatricsnationwide.org/wp-content/themes/corpus/images/empty/thumbnail.jpg 150 150 Abbie Miller Abbie Miller https://pediatricsnationwide.org/wp-content/uploads/2023/05/051023BT016-Abbie-Crop.jpgRhabdomyosarcoma with breast involvement is found almost exclusively in females. A recent case series highlights the need for guidelines for follow-up imaging.
Rhabdomyosarcoma (RMS) is a soft tissue sarcoma associated with metastasis and inferior outcomes in adolescent and young adult (AYA) patients (those with cancer diagnosis at age 15-39 years). Metastases to the breast have been reported in 3 to 6 percent of RMS patients.
“RMS metastases to the breast are not common, and not surprisingly, they have been reported almost exclusively in females,” says Anthony Audino, MD, pediatric oncologist in Hematology/Oncology & Blood and Marrow Transplant at Nationwide Children’s Hospital. “Metastatic RMS carries a dismal prognosis overall, and breast involvement often occurs in the context of widely metastatic disease.”

In a case series review recently published in the Journal of Pediatric Hematology and Oncology, Dr. Audino and his colleagues reviewed cases of RMS in the Nationwide Children’s Hospital Tumor Registry between January 1, 2004 and December 31, 2013. The series demonstrated breast involvement in 8.7 percent of all RMS patients in the cohort, which is similar to previous reports.
The team identified four cases of RMS with breast involvement among the ten AYA females in the cohort. All four patients with breast involvement had alveolar RMS, which has been reported to be the most common histologic variant involving the breast. Notably, three of the four patients also had bone marrow involvement, though a correlation has not been reported elsewhere in the literature.
Little data is available to guide the management of primary or metastatic breast RMS, particularly in the AYA population. In general, surgical resection of the primary tumor with complete margins is preferred when possible; however, a range of surgical approaches, from lumpectomy to radical mastectomy, have been reported.
“The psychosocial implications of a mastectomy are well documented in the adult literature, with females having significant body image issues, as well as physical and emotional distress following aggressive surgeries,” explains Dr. Audino. “One may argue that the risk of such psychosocial implications and stressors may be heightened in adolescents and young adults, where body image already plays such a large role in the social environments that they encounter. The ramifications of this intervention should be balanced by an overall consideration of the patient’s prognosis.”
The clinical impact of these findings for young women with RMS is not established. While routine imaging of the breasts in young women with RMS has been suggested, it is not currently standard practice at diagnosis or in follow up.
At diagnosis, many patients will have computed tomography (CT) of the chest performed as well as whole-body positron emission tomography (PET) imaging, abrogating the need for specific breast imaging, according to Dr. Audino, who is also assistant professor of Pediatrics at The Ohio State University College of Medicine.
“Routine breast exam as part of the follow-up process is currently not a recommendation, although it would seem prudent,” says Dr. Audino. “Particularly for adolescent females with alveolar histology or extremity primary tumors.”
Further research is needed to better understand RMS in the AYA population. Following the results of this paper, Dr. Audino and his team will be developing a standard of care regarding work-up and follow-up imaging, with an emphasis on AYA women with RMS.
Reference:
Audino AN, Setty BA, Yeager ND. Rhabdomyosarcoma of the breast in adolescent and young adult (AYA) women. Journal of Pediatric Hematology and Oncology. 2017 Jan;39(1):62-66.
Photo credit: Adobe Stock
About the author
Abbie (Roth) Miller, MS, MWC, is a passionate communicator of science. As the manager of medical and science content at Nationwide Children’s Hospital, she shares stories about innovative research and discovery with audiences ranging from parents to preeminent researchers and leaders. She is a Medical Writer Certified®, credentialed by the American Medical Writers Association, and received her masters of science in Health Communication from Boston University.
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Post Tags:
- Hematology/Oncology/BMT
- Posted In:
- In Brief