Pediatric Vital Signs: Measuring and Improving the Health of a Population
Pediatric Vital Signs: Measuring and Improving the Health of a Population https://pediatricsnationwide.org/wp-content/themes/corpus/images/empty/thumbnail.jpg 150 150 Jeb Phillips Jeb Phillips https://pediatricsnationwide.org/wp-content/uploads/2021/03/Jeb-Phillips.jpgNationwide Children’s Hospital and its community partners have begun an “audacious” project to help every child in their region.
Despite the best efforts of primary care providers and children’s hospitals, some children do not receive the care they need. Patients can only spend a limited amount of time in a medical office; some who would benefit the most may not come in at all.
Nationwide Children’s Hospital, like many other institutions, has wrestled with those obstacles for years. In the words of Kelly Kelleher, MD, MPH, the hospital’s vice president of Community Health, Nationwide Children’s has wanted to adjust its perspective “from health care to health,” or from a focus on the delivery of individual services to a focus on population-level wellbeing.
This is part of the motivation behind Partners For Kids®, Nationwide Children’s accountable care organization, which uses quality improvement, care coordination and other programs to help 400,000 children covered by Medicaid managed care in Ohio. It’s also driven the Healthy Neighborhoods Healthy Families initiative, which uses high-quality housing, workforce training, student mentorship and other methods to improve some of Columbus, Ohio’s most at-risk neighborhoods.
These are important moves toward population health, but they still can’t reach an entire region’s children. So what could? How could every child’s health be accounted for and improved?
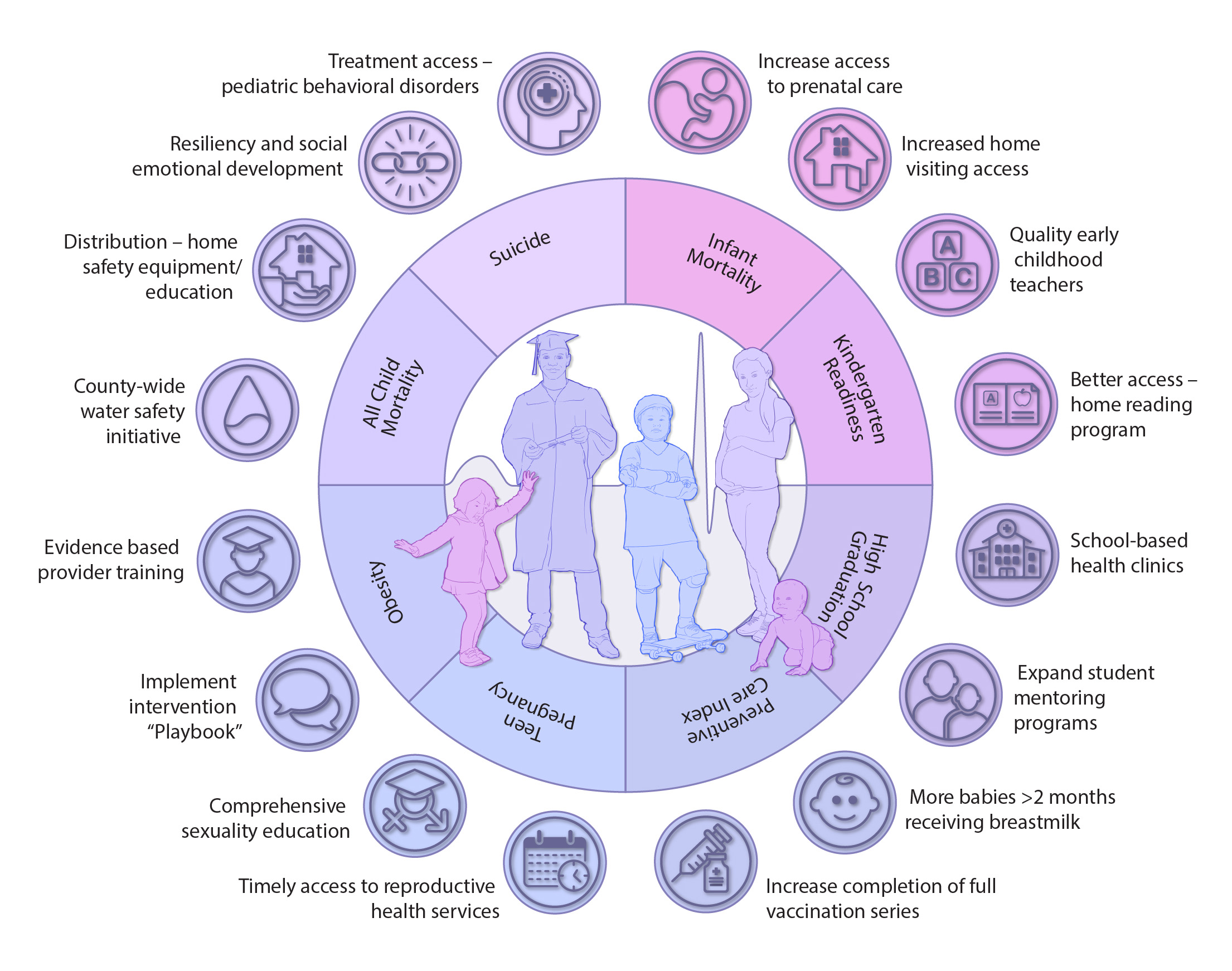
That is the audacious goal of Nationwide Children’s Pediatric Vital Signs project. In the same way that traditional vital signs such as temperature and blood pressure give an indication of an individual child’s health, Pediatric Vital Signs is an effort to meaningfully measure the wellbeing of all children in Franklin County, Ohio across eight metrics that span childhood. That mindset is being used to define and implement interventions to improve overall outcomes, regardless of where or how children receive health care.
These metrics are: infant mortality, kindergarten readiness, high school graduation, obesity, teenage pregnancy, suicide, all-cause child mortality and a hybrid measure called preventive services delivery (including measurements of lead screening, primary vaccination series, breastfeeding and various behavioral and physical health screenings).
Some of the metrics, such as kindergarten readiness and high school graduation rates, aren’t even strictly health care-related – but they do impact a child’s life and health. All of the metrics have elements of racial and ethnic disparity that must be addressed. All need a broad coalition of stakeholders, including public health officials, schools, non-profit agencies, civic organizations and local governments, to come together to make a difference.
“We don’t want to restrict ourselves to what would be easy, or what could just be accomplished by a children’s hospital acting alone,” says Alex Kemper, MD, MPH, MS, division chief of Primary Care Pediatrics at Nationwide Children’s, professor of Pediatrics at The Ohio State University and lead author of a commentary piece in the Journal of Pediatrics introducing Pediatric Vital Signs. “We are deeply committed to ‘health,’ with every meaning of that word. A children’s hospital has the resources to be able to lead, but it takes everyone.”
Choosing the Pediatric Vital Signs
In 2015, the National Academy of Medicine (NAM) introduced a set of 15 standardized core metrics that could be used to evaluate the country’s health, and they mirrored and helped shape the thinking of Dr. Brilli, Dr. Kelleher and their team. NAM called the metrics “Vital Signs.” Many of those signs seemed tailored for adult health, but the overall concept made sense to use as a model, so Nationwide Children’s called its project “Pediatric Vital Signs.”
“We have a whole population health infrastructure with Partners For Kids, with Healthy Neighborhoods Healthy Families, our school-based health programs and so much more,” says Dr. Kelleher. “They all feed this vision of ‘Best Outcomes’ for everyone. They all roll up into what we wanted for Pediatric Vital Signs.”
One of the greatest challenges was selecting the signs, says Dr. Brilli. They all needed to be relevant to large numbers of children across the entire period of childhood, so that improving any of them would mean a broad improvement across the population. They also must be measurable, with reliable data underlying any interventions, just as with the infant mortality efforts.
Over the course of 15 months, the Pediatric Vital Signs team chose the eight metrics, all of which have lifelong implications. The team also developed or gathered ways to measure the signs; created individual teams to address them, including external community partners; chose ambitious improvement goals for 2020, 2025 and 2030; and identified interventions to achieve each goal, spelled out through a series of key driver diagrams.

Some of the Pediatric Vital Signs, such as infant mortality, have years of collaboration and intervention already pointing the way to the future. Some, such as high school graduation, have only scratched the surface. But what happens from here on is clear.
“We’ve done all this work to build coalitions. We developed the signs,” says Sander. “Now we have to execute.”
The Future and Why Other Regions Should Monitor Their Own Pediatric Vital Signs
The COVID-19 pandemic and this year’s spotlighting of racism and racial inequities have only emphasized the importance of Pediatric Vital Signs.
“We now have these measures that will help us know exactly where kids are falling behind — in immunizations, in kindergarten readiness, in all of the other areas — and allow us to creatively develop ways to catch them up,” says Dr. Kemper. “Social determinants of health and racial disparities have always been built into the Pediatric Vital Signs work, and we can only be successful if we’re successful in addressing them.”
The national events of 2020 have heightened the national appetite for measures like Pediatric Vital Signs, says Benard Dreyer, MD, director of the Division of Developmental and Behavioral Pediatrics at NYU Langone Health and a past president of the American Academy of Pediatrics.
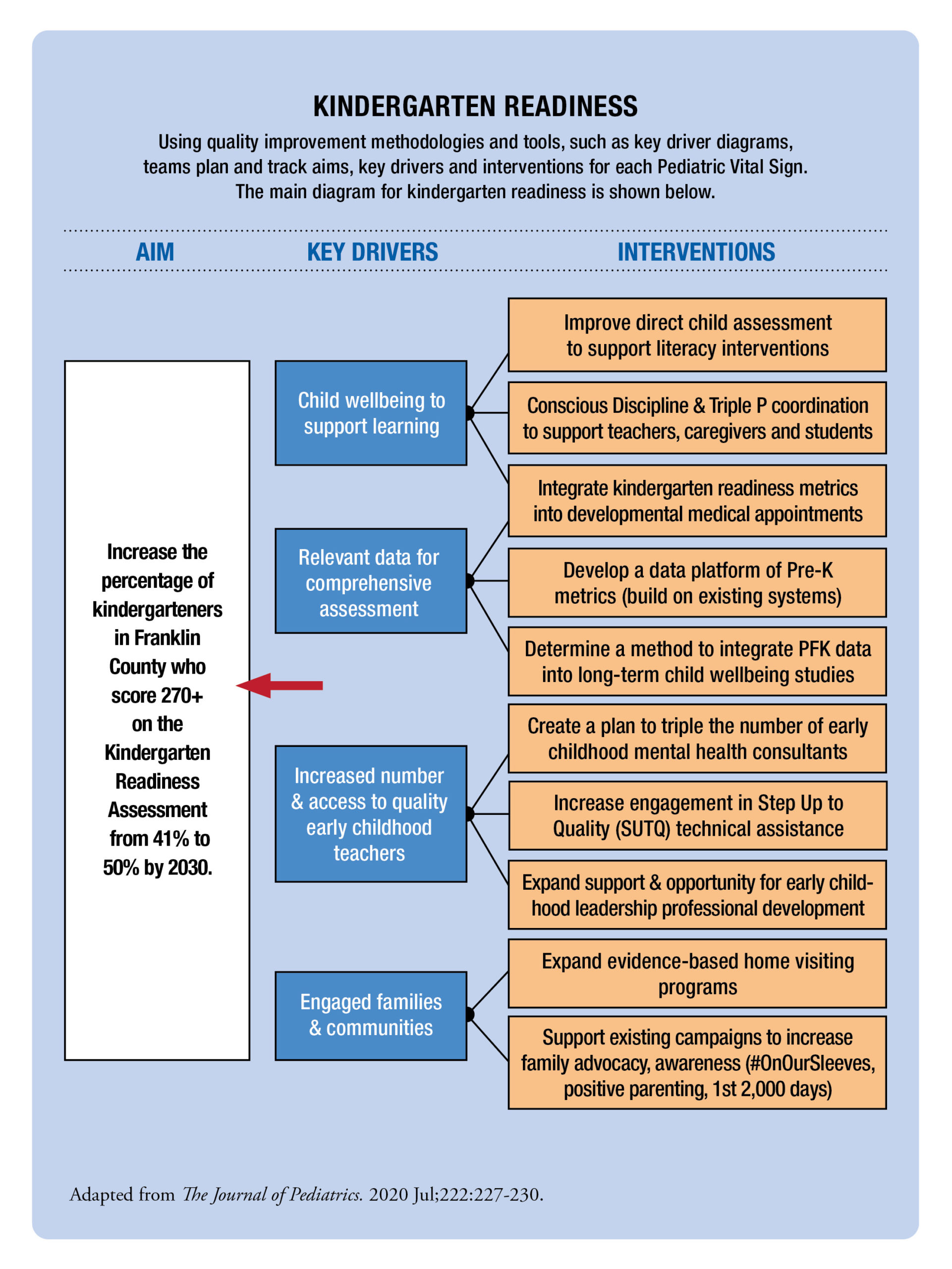
“As an example, we know that for children not ready to start school because of poor self-regulation and basic skills, it’s very difficult to make up that difference later,” he says. “Children who are behind in kindergarten are likely going to be behind in fifth grade and eighth grade. If you could really do something for kindergarten readiness, it would do a lot for the trajectory of a child’s life.”
The issue, Dr. Dreyer says, is so many of the Pediatric Vital Signs represent what are considered “intractable problems.” Too big, too complicated.
“If you can get the right people in the right coalitions and show that you can move the needle, that would be a great stimulus to other people throughout the country,” he says.
Along with improving the wellbeing of children in central Ohio, inspiring others is a primary goal of Pediatric Vital Signs, according to Dr. Brilli. Such an enormous project can seem paralyzing, but Nationwide Children’s hopes to show that it’s possible – and that a children’s hospital, with a service mission and deep community goodwill, is the perfect organization to make it happen.
Eight vital signs may be too many for some to take on at first, Dr. Brilli says. Other signs may fit a certain region better than the ones Nationwide Children’s has chosen. The important thing is to make the effort.
“I’m not daunted. In fact, I’m inspired,” Dr. Brilli says. “We don’t have it all figured out. But think how much of an impact this could have to help every child achieve their full potential.”
This story appeared in the Fall/Winter 2020 print issue. Download the issue now.
Reference:
Kemper AR, Kelleher KJ, Allen S, Sander C, Brilli RJ. Improving the health of all children in our community: the Nationwide Children’s Hospital and Franklin County, Ohio, Pediatric Vital Signs project. The Journal of Pediatrics. 2020 Jul; 222:227-230.
Image Credit: Nationwide Children’s
About the author
Jeb is the Managing Editor, Executive Communications, in the Department of Marketing and Public Relations at Nationwide Children's Hospital. He contributes feature stories and research news to PediatricsOnline, the hospital’s electronic newsletter for physicians and other health care providers, and to Pediatrics Nationwide. He has served as a communications specialist at the Center for Injury Research and Policy at The Research Institute and came to Nationwide Children’s after 14-year career as daily newspaper reporter, most recently at The Columbus Dispatch.
- Jeb Phillipshttps://pediatricsnationwide.org/author/jeb-phillips/
- Jeb Phillipshttps://pediatricsnationwide.org/author/jeb-phillips/
- Jeb Phillipshttps://pediatricsnationwide.org/author/jeb-phillips/November 24, 2015
- Jeb Phillipshttps://pediatricsnationwide.org/author/jeb-phillips/
- Posted In:
- Features







