Fetal Balloon Aortic Valvuloplasty for Critical Aortic Stenosis
Fetal Balloon Aortic Valvuloplasty for Critical Aortic Stenosis https://pediatricsnationwide.org/wp-content/uploads/2019/04/Insight-Left-Side_FINAL-for-web-header-1024x575.jpg 1024 575 Abbie Miller Abbie Miller https://pediatricsnationwide.org/wp-content/uploads/2023/05/051023BT016-Abbie-Crop.jpg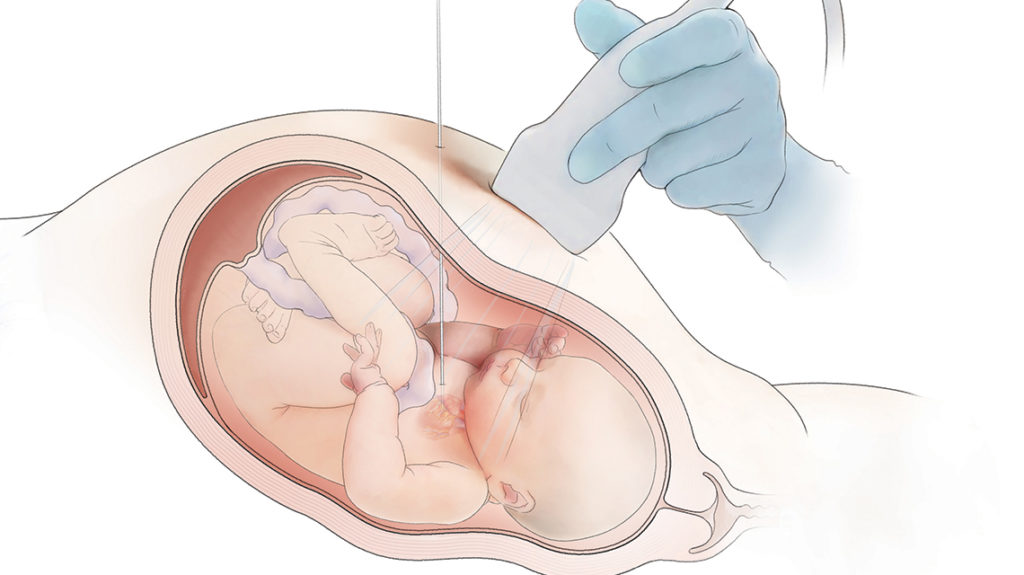
Some heart defects, such as aortic stenosis can be detected on fetal ultrasound. For some fetuses, an intervention can be beneficial before birth. Aimee Armstrong, MD, director of Cardiac Catheterization and Interventional Therapies at Nationwide Children’s Hospital, performs fetal balloon aortic valvuloplasty among other fetal heart catheterization procedures as part of the Congenital Heart Collaborative, a partnership between University Hospital’s Rainbow Babies and Children’s and Nationwide Children’s.
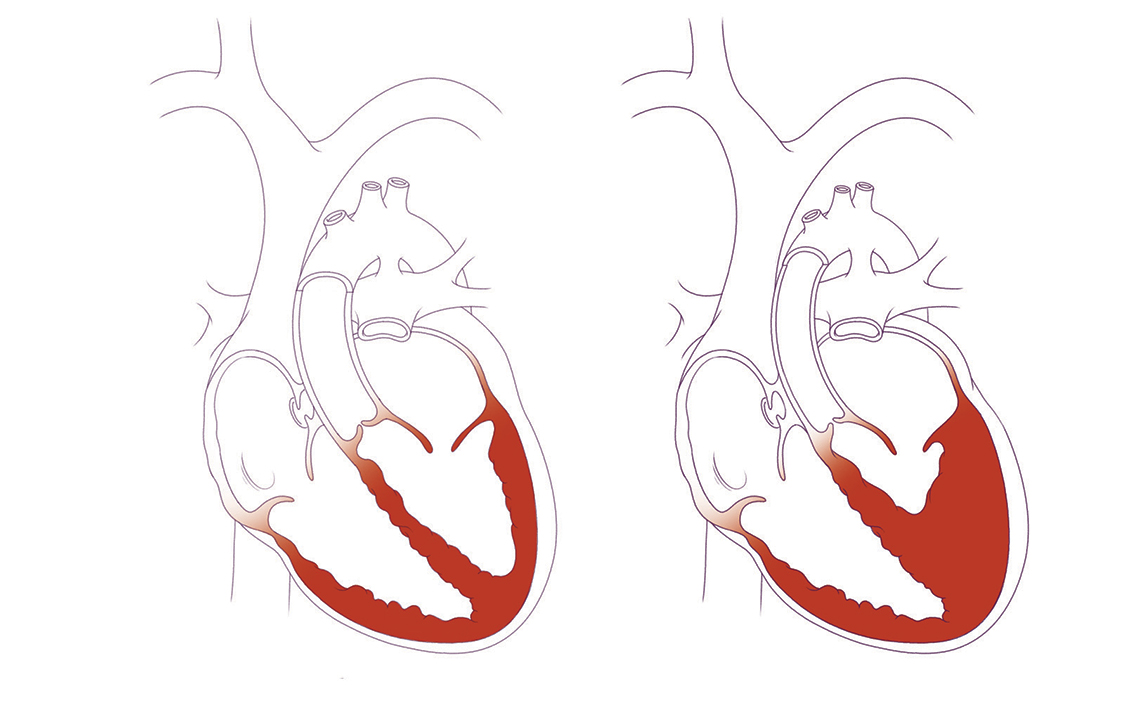
When critical aortic stenosis is present in a second trimester fetus, the left ventricle becomes enlarged and weak. As a result, there is less blood flow through the left side of the heart. This can cause the left ventricle to stop growing, leading to hypoplastic left heart syndrome (HLHS). Through fetal treatment of the critical aortic stenosis, doctors hope to prevent the formation of HLHS.
In HLHS, the left side of the heart is underdeveloped. Patients with HLHS have one pumping chamber that must send blood to both the lungs and the body. This causes both short- and long-term problems, including many open-heart surgeries, catheterization procedures, and, eventually, heart transplantation.
The Procedure
First, the mother has an epidural placed. Then, a needle is used to provide pain medicine to the fetus through an injection in the thigh.
Next, a needle is inserted into the mother’s abdomen and uterus, through the fetus’s ribs and into the fetus’s heart.
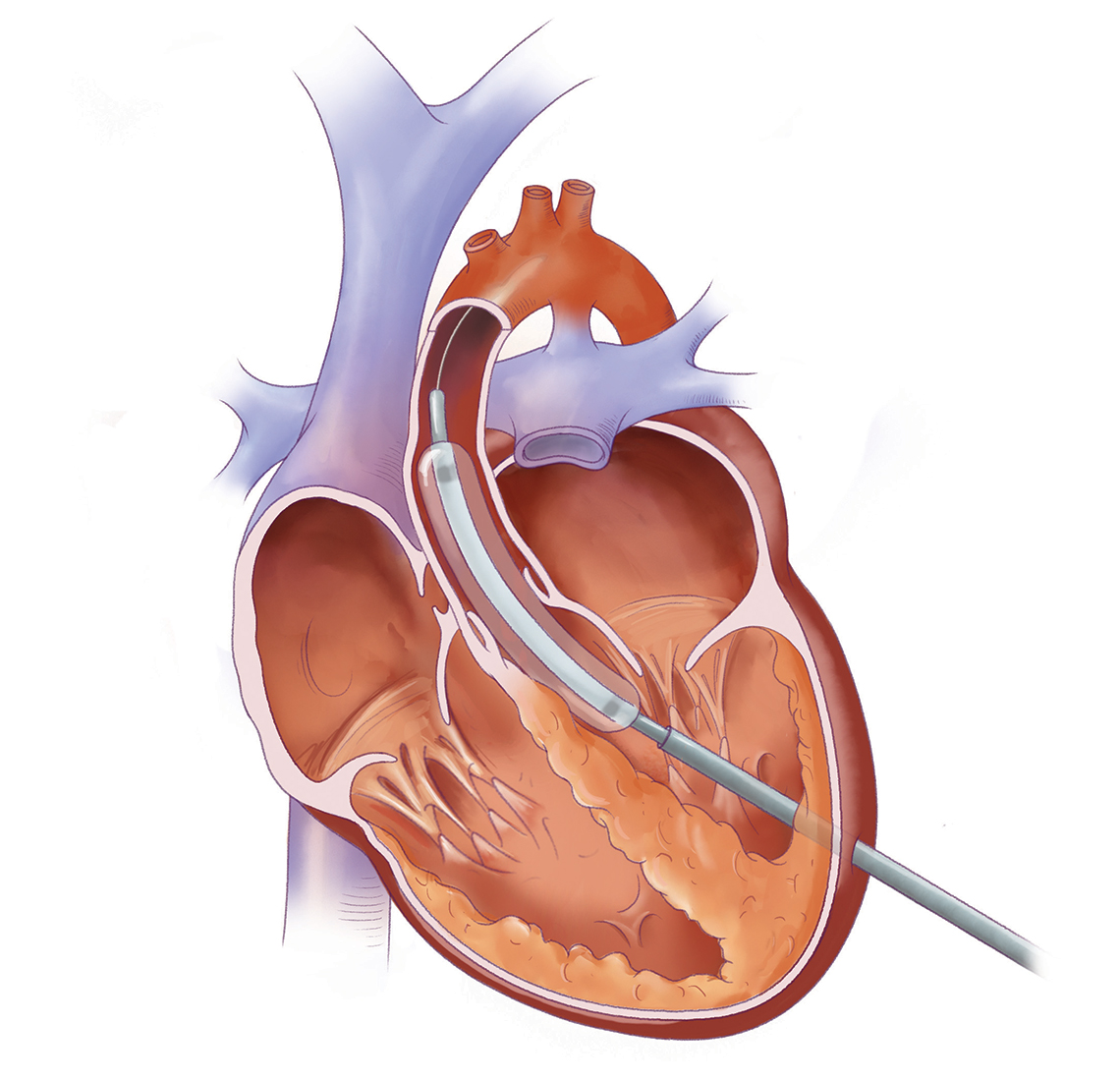
A wire and tiny coronary angioplasty balloon are placed through the needle across the aortic valve. The balloon is then gently inflate to make the opening of the aortic valve bigger. The balloon, wire and needle are then removed.
After the procedure, doctors watch the mother and baby with many fetal ultrasounds an fetal echocardiograms. The goal is for the mother to deliver as close to full term as possible.
About the author
Abbie (Roth) Miller, MS, MWC, is a passionate communicator of science. As the manager of medical and science content at Nationwide Children’s Hospital, she shares stories about innovative research and discovery with audiences ranging from parents to preeminent researchers and leaders. She is a Medical Writer Certified®, credentialed by the American Medical Writers Association, and received her masters of science in Health Communication from Boston University.
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/







