The Evolution of Precision Medicine for Children With Aggressive Brain Tumors
The Evolution of Precision Medicine for Children With Aggressive Brain Tumors https://pediatricsnationwide.org/wp-content/themes/corpus/images/empty/thumbnail.jpg 150 150 Jonathan Finlay, MB, ChB, FRCP Jonathan Finlay, MB, ChB, FRCP https://pediatricsnationwide.org/wp-content/uploads/2021/03/113016ds1231-finlay-bio.gifThe Head Start 4 clinical trial introduces risk stratification and builds on the success of bone marrow transplantation for young children with malignant embryonal tumors.
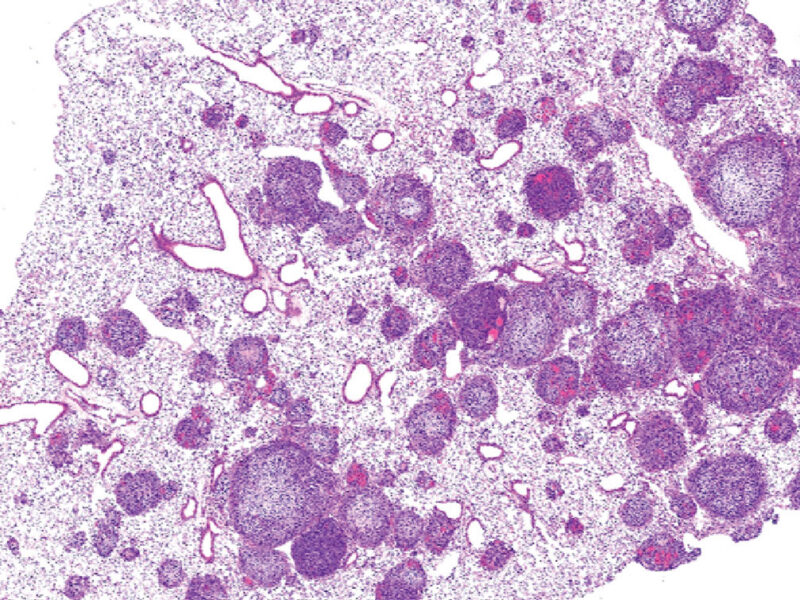
Cancers in the brain and spinal cord (the central nervous system, CNS) are now the most common cause of deaths due to disease in children and adolescents. Among these tumors, the most common malignant kind in childhood are embryonal tumors. These tumors are masses of rapidly growing cells that begin in embryonal (fetal) tissue and include medulloblastoma and pineoblastoma, among others. They develop most frequently in children under 6 years of age.
While the overall survival of children with CNS cancers in the last two decades has seen significant improvments, outcomes are especially uncertain for young children with malignant embryonal brain tumors. First, the tumors tend to behave more aggressively in young children. Second, the side-effects of traditional radiation therapy in addition to drug therapy are toxic to the developing brain of young children, leaving severe and irreversible damage with profound effects upon learning, development and overall quality of life.
In 1991, the accumulating evidence of brain damage caused by radiotherapy in young children led to a novel approach in North America, called the Head Start program. Since then, three successive ”Head Start” treatment studies conducted among pediatric cancer centers throughout the United States, Canada, Australia, Argentina, New Zealand and Switzerland have moved science forward to improve outcomes for children with CNS tumors.
The strategy in these studies has been to avoid radiotherapy through the use of highly-intensive drug therapy. This therapy concludes with a single cycle of marrow-destructive chemotherapy with rescue by a bone marrow or blood cell transplant of the child’s own (previously collected and preserved) cells. These studies have successively documented increasing cancer-free survival, with decreasing side-effects and preserved long term normal quality of life.
The Head Start 3 study was completed in December 2009, and the long-term outcomes have been published over the last few years, enabling us to build on the prior studies.
In mid-2015, the Head Start 4 study was started at Nationwide Children’s Hospital in order to test a new strategy. As of September 2017, 27 institutions throughout North America have opened the study to patient participation, and we are currently enrolling 2-3 children each month as an additional 20 or so institutions throughout North America, Australia, and New Zealand begin participating.
So what’s different about Head Start 4? It is the first study in young children to use molecular information of each child’s tumor to assign them to either a standard-risk or a high-risk group. Children in the standard-risk group may be able to receive less-intensive chemotherapy compared with prior Head Start studies because of their excellent outcomes. Children with high-risk tumors, after initial drug therapy to reduce their tumor burden, will be randomized to receive either the standard single-cycle blood cell transplant regimen or a regimen of three sequential blood cell transplants, to test whether the latter will improve the outcomes for these children.
The Head Start 4 study is directed through the NEXT Consortium in the Clinical Research Office of the Division of Hematology, Oncology & Blood and Marrow Transplantation at Nationwide Children’s Hospital.
About the author
Jonathan L. Finlay, MB, ChB, FRCP is the program director of Neuro-Oncology at Nationwide Children’s Hospital. Dr. Finlay is a tenured professor of Pediatrics at The Ohio State University College of Medicine. He is an internationally recognized expert in pediatric brain tumors and has authored or co-authored over 200 peer-reviewed publications in leading medical journals and over 80 review articles and book chapters.
- Post Tags:
- Hematology/Oncology/BMT
- Neuro-Oncology
- Posted In:
- In Brief