Creating a Physician Workforce that Reflects the Patients and Families We Serve
Creating a Physician Workforce that Reflects the Patients and Families We Serve https://pediatricsnationwide.org/wp-content/uploads/2021/11/071919ds9080-web-1024x683.jpg 1024 683 Abbie Miller Abbie Miller https://pediatricsnationwide.org/wp-content/uploads/2023/05/051023BT016-Abbie-Crop.jpg
Workforce disparities persist within health care institutions and medical training. While individuals who identify as Black/African American, Latinx/Hispanic, Native American, and Pacific Islander comprise roughly 30% of the U.S. population, they are less than 15% of physicians, making them underrepresented in medicine – or URM. In fact, as the U.S. population grows more diverse, the racial and ethnic demographic gap between patients and physicians, including pediatricians, is worsening.
In a bold effort to bridge that gap, a team of physicians (medical educators, advocates and researchers) at Nationwide Children’s Hospital developed a plan. The plan and its results are now published in Pediatrics.
“We aspired to develop more effective strategies for recruitment of URM students into our residency program,” says Monica Hoff, MD, chief resident at Nationwide Children’s. “We hypothesized that disparities in our training programs might be perpetuated by the premise that, ‘You can’t be what you can’t see,’ as stated by children’s rights activist Marian Wright Edelman. In short, we believed that URM recruitment would increase if applicants were exposed to physicians with whom they could identify, illustrating a culture of inclusive excellence.”
The team’s aim was to increase the percentage of URM residents who matched into the Pediatric, Child Neurology, and Medical Genetics residency programs from a baseline of 5% to 35%, achieving demographic parity with the hospital’s patient population.
Through implementing small, low-resource strategies that had a large cumulative impact, the percent of URM residents who matched increased from 5% to 16% in 2018, 26% in2019, 19% in 2020 and 21% in 2021.
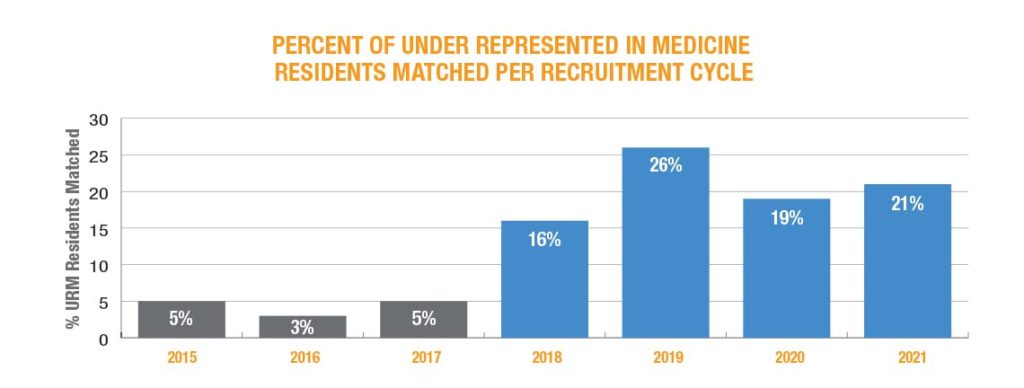
Some of the strategies implemented during the first four residency recruitment cycles of this project include:
- Increasing visibility of URM faculty during recruitment interviews
- Implicit bias training for all residency program directors
- Creation of a visiting student elective for fourth year URM medical students
- Increased involvement and visibility of URM residents in interview dinners
- Increasing visibility of diverse workforce in marketing materials (print and digital) and social media channels
During the 2019-2020 recruitment year, our URM Resident Recruitment Task Force transitioned to a more robust resident-led minority house staff organization (MHO), named the Resident Diversity Inclusion Coalition, which was expanded to include Lesbian, Gay, Bisexual, Transgender, Queer (LGBTQ) faculty and trainees. MHO members became standing members of the Pediatric Residency Recruitment Committee.
The authors also describe the actions taken to address the “minority tax” in the implementation of the plans.
“The expectation that minority trainees and faculty take on additional responsibility by participating in diversity initiatives—the minority tax—can result in competing responsibilities for residents and faculty,” says Dr. Hoff. “Unfortunately, the more interventions that we added to increase the visibility of URM residents and faculty, the more duties were added to their workload, but there are a number of ways to mitigate the minority tax.”
Increasing the number of URM faculty and residents helped to offset some of that tax, the authors report. However, it is not a solution to the problem.
“The best way to mitigate the minority tax is a robust institutional, faculty and graduate medical education commitment to diversity and equity,” says Ray Bignall, MD, pediatric nephrologist and assistant chief diversity and health equity officer at Nationwide Children’s and the publication’s senior author. “In an ideal scenario, these responsibilities are shared by everyone in the recruitment, training, and retention processes – not only these team members from minoritized groups. Furthermore, these efforts should be supported by institutional leaders with capital investments, as well as faculty and staff FTEs.”
A workforce that reflects the patient population is associated with improved patient outcomes. “Creating just, equitable, diverse, and inclusive spaces for our patients, families, and staff is foundational to our vision of excellence in compassion, healing, discovery and innovation at Nationwide Children’s,” adds Dr. Bignall. “It doesn’t matter if our patients are from Linden, Lima, or Los Angeles; from the West Side, West Virginia, or West Africa. Championing diversity and health equity is how we prove that every child, every family, and everyone matters here.”
Reference:
Hoff ML, Liao NN, Mosquera CA, Saucedo A, Wallihan RG, Walton JR, Scherzer R, Bonachea EM, Thomas OW, Mahan JD, Barnard JA, Bignall II ONR. Results and reflections on a successful initiative to increase residency program diversity. Pediatrics. 2021.
Image credit: Nationwide Children’s
About the author
Abbie (Roth) Miller, MS, MWC, is a passionate communicator of science. As the manager of medical and science content at Nationwide Children’s Hospital, she shares stories about innovative research and discovery with audiences ranging from parents to preeminent researchers and leaders. She is a Medical Writer Certified®, credentialed by the American Medical Writers Association, and received her masters of science in Health Communication from Boston University.
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Post Tags:
- Health Equity
- Residency
- URM