Simulating Surgery With High-Performance Computing
Simulating Surgery With High-Performance Computing https://pediatricsnationwide.org/wp-content/uploads/2016/04/Back-Cover-Art-1024x575.jpg 1024 575 Abbie Miller Abbie Miller https://pediatricsnationwide.org/wp-content/uploads/2023/05/051023BT016-Abbie-Crop.jpg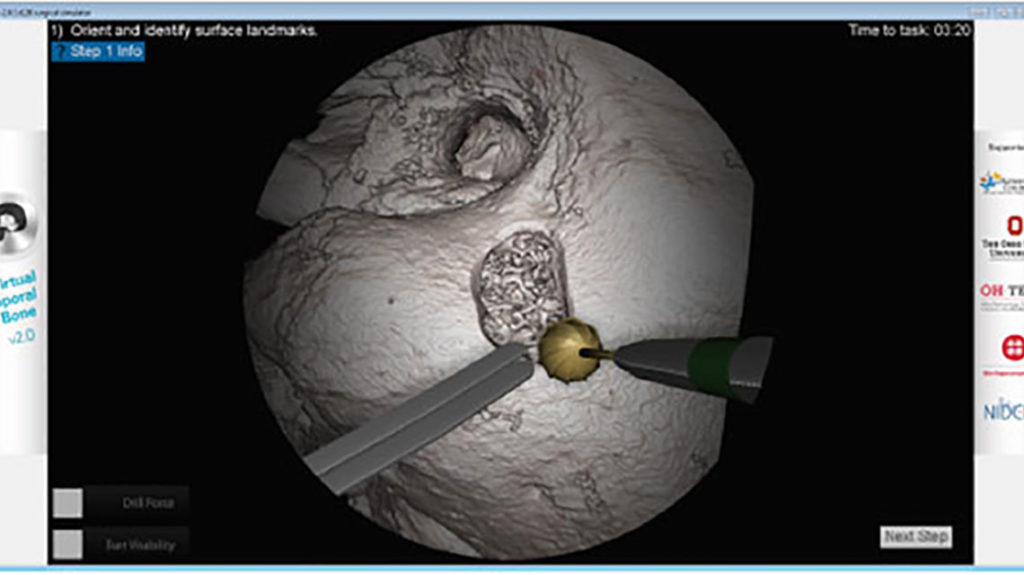
By applying high-performance computing to the field of otolaryngology, a team of researchers is developing a simulation environment for teaching surgical techniques related to the temporal bone.
The purpose of training — whether a fire drill or practicing a surgical technique — is to create successes and avoid failures.
“The impact of training is safety and lives saved,” says Gregory J. Wiet, MD, otolaryngologist and principal investigator at Nationwide Children’s Hospital. By creating a robust, high-fidelity, interactive temporal bone surgical simulation system, Dr. Wiet and his team are on the forefront of using high-performance computing to improve surgical education and training. The NIH-funded project is breaking new ground for otolaryngologists, neurosurgeons and others who are training to operate on this delicate anatomy.
According to Dr. Wiet, temporal bone surgery is among the most complex and technically challenging in the field of medicine. Training surgeons to operate in this area is a challenge for the medical community, which currently relies on books, cadaver dissection and observation of more experienced surgeons with gradual transfer of responsibility.
“When we embarked on this challenge, our objective was to improve the efficiency of training and assessment of technical skill in the surgical treatment of otologic disease,” says Dr. Wiet. “We believe that a properly designed and validated temporal bone surgical simulator will accomplish this.”
Dr. Wiet’s multidisciplinary team includes specialists from
- Biomedical Applications Research Group at The Ohio State University/Ohio Super Computing
- Image data acquisition
- Biomedical engineering
In 2012, Dr. Wiet and his team validated their temporal bone simulation against cadaveric dissections, proving that the method was an effective training tool. Since then, they have further refined the system, including more advanced scoring metrics, haptic feedback and image resolution. The system includes 40 different simulated bones, and the team is currently incorporating the data for a neonatal skull.
“Simulation technology provides technical skills training in the midst of safe and efficient patient care, flexibility to handle changes in specific skills training and development of new techniques, and standardized and objective assessment of technical skills,” says Dr. Wiet, who is also professor of Otolaryngology, Pediatrics and Biomedical Informatics and director of Pediatric Otolaryngology Research at The Ohio State University College of Medicine. “It is also valuable as a means of realistic presurgical planning and rehearsal.”
The current system supports complete mastoidectomy with automated metrics. Once a procedure or training exercise is completed, users receive immediate feedback in the form of a score, which has been calculated based on a rubric ranking the specific points of the procedure. Advances are underway including fidelity to support higher level procedures, fluid simulation and additional standardized metrics.
“A national consortium of 13 institutions is using and testing the simulations. This collaboration gives institutions access to the software, while we have access to more residents to test the software and provide feedback,” says Dr. Wiet. “This involvement contributes to making our program the most advanced of its kind.”
About the author
Abbie (Roth) Miller, MS, MWC, is a passionate communicator of science. As the manager of medical and science content at Nationwide Children’s Hospital, she shares stories about innovative research and discovery with audiences ranging from parents to preeminent researchers and leaders. She is a Medical Writer Certified®, credentialed by the American Medical Writers Association, and received her masters of science in Health Communication from Boston University.
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Post Tags:
- Otolaryngology
- Research
- Surgery
- Posted In:
- Features