From Expectant Parents to Advocates: One Family’s Journey With Hypoplastic Left Heart Syndrome
From Expectant Parents to Advocates: One Family’s Journey With Hypoplastic Left Heart Syndrome https://pediatricsnationwide.org/wp-content/uploads/2020/07/050420BS0147G-mila-header-1024x575.jpg 1024 575 Abbie Miller Abbie Miller https://pediatricsnationwide.org/wp-content/uploads/2023/05/051023BT016-Abbie-Crop.jpg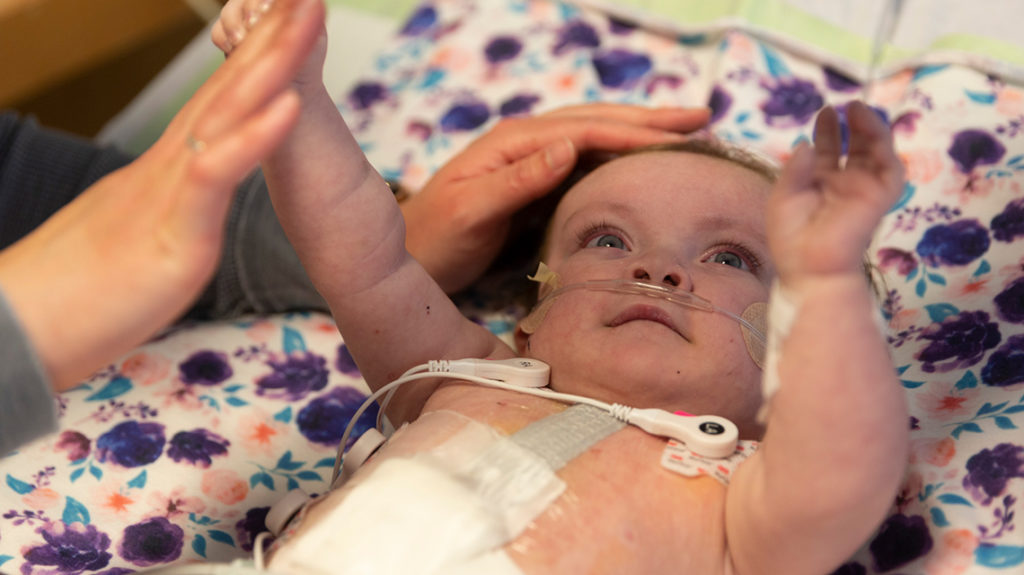
Mila’s parents wanted her to have the best chance at surviving her high-risk comprehensive stage 2 surgery – their journey led them to The Heart Center at Nationwide Children’s.
Mid-way into their pregnancy, Jacob and Kayla went in for their 20-week ultrasound.
“We were very excited to get into things like paint colors for our daughter,” says Jacob. “And then we found out that there was a possible abnormality in the left side of our daughter’s heart.”
At a 22-week ultrasound, their fears were confirmed: their daughter had hypoplastic left heart syndrome (HLHS).
As Jacob and Kayla started to think about the realities of their daughter’s care, they felt fortunate that a hospital only 40 minutes from their home in Iowa had a great reputation.
After Mila was born, she had some complications that resulted in a prolonged initial hospital stay of 96 days. During that time, she underwent the hybrid stage 1 palliation.
Hybrid vs Norwood
Most infants with HLHS or other congenital heart defects resulting in a single ventricle undergo the Norwood operation as the first of three operations in this care path. This traditional approach front loads the greatest mortality risk to the first operation, and subsequent surgeries pose minimal risk to patients. An alternative approach, called the hybrid, also has three expected operations in the care path. But the hybrid approach begins with hybrid stage 1 palliation, which offers a less invasive, lower risk initial surgery and puts off the more complex operation until the patient is 4 to 6 months old — ideally, larger, healthier and better equipped to recover from the complex surgery. The hybrid approach reduces the cumulative risk of serious complications and death.
“At most pediatric heart centers around the country, the hybrid procedures are only considered if the patient is very high risk for the Norwood,” says Mark Galantowicz, MD, chief of Cardiothoracic Surgery and co-director of The Heart Center, and co-inventor of the hybrid procedure. “They view hybrid stage 1 as a rescue procedure. For those that survive, the patients end up needing a comprehensive stage 2 operation in a center that has done very few of them.”
In The Heart Center at Nationwide Children’s, the hybrid procedure is the preferred approach to treating HLHS. This means that surgeons at Nationwide Children’s do far more stage 2 procedures than surgeons in other centers.
As Jacob and Kayla started to look into Mila’s next procedure – the comprehensive stage 2 – they were discouraged at the high mortality rates. But they also noticed that the rates at Nationwide Children’s Hospital were better than average. They discovered, as well, that many of the publications about this procedure were being published by Dr. Galantowicz, chief of Cardiothoracic Surgery and Co-director of The Heart Center at Nationwide Children’s.
“With the comprehensive stage 2 procedure, there’s a learning curve. Our research and analysis show that it takes doing the procedure about 10 to 12 times for a surgical team to become competent across the board,” explains Dr. Galantowicz. “In centers that only do hybrids as a back-up plan, it’s hard to achieve those volumes.”
Dr. Galantowicz and his team have performed almost 200 comprehensive stage 2 procedures.
From Iowa to Ohio
“After learning all of this, it became really important for us to have Mila’s surgery done by the most experienced team we could find – Nationwide Children’s,” says Jacob. “The team at the hospital in Iowa was extremely supportive in helping us with the transfer request. They even wrote the referral for the insurance company.”
The first transfer request was denied by the insurance company very quickly, the peer-to-peer review (in which an insurance company’s medical director or medical staff discusses the request with the requesting physician) coming back in less than 45 minutes. And then there was a second rejection.
Jacob says, “From a parental standpoint it doesn’t sit well when you have a huge decision to make and along the way you respect all the rules and do all the legwork and then you don’t get to advocate for your own child.”
They requested the transfer a third time, following insurance guidelines to appeal. They crafted a letter detailing the case history and why they found it medically necessary to transfer to a hospital that has proven, positive results.
“It was important for us to pick up the fight on behalf of our daughter and present our rationale for making sure she was put into the situation that was best for her,” says Jacob. “We were ecstatic when our insurance company approved!”
Once the transfer was approved, everything moved quickly. The approval came on a Thursday, and Mila was in surgery at Nationwide Children’s early the following week.
Despite the fact that his daughter was having a major open-heart surgery, Jacob says he felt relieved. “I felt like a huge weight had been lifted and the anxiety almost disappeared. She was still going into surgery and we were worried, but I knew she was at the right place.”
Dr. Galantowicz and his team also supported the family as they negotiated the request for transfer process.
“The pace of innovation can create knowledge gaps, even at the level of medical director of an insurance company,” he says. “It’s important and appropriate for parents to advocate for their children, especially for unique cases and rare conditions, such as HLHS.”
Mila’s surgery at Nationwide Children’s went well, and she is now home with her family.
“We are incredibly thankful for Dr. Galantowicz and the team’s expertise and compassion,” says Jacob. “This surgery allowed Mila to survive. And now we have a long-term care plan, too.”
A Path Forward for Sharing Surgical Innovation
So if it takes 10 to 12 procedures to develop competency, how can surgeons across the country gain the necessary experience to improve the level of care offered for patients?
“This is an important question for our field,” says Dr. Galantowicz. “And one that is not easily answered. In heart programs across the country, different programs develop expertise in different areas – a procedure, a disease variation. It’s essential that we remember that it is okay to refer or ask for a consultation if that is in the best interest of the patient.”
To read more about Mila’s story, visit flutter.nationwidechildrens.org/mighty-mila.
Image credit: Nationwide Children’s
Melisa Wells contributed to this story.
About the author
Abbie (Roth) Miller, MS, MWC, is a passionate communicator of science. As the manager of medical and science content at Nationwide Children’s Hospital, she shares stories about innovative research and discovery with audiences ranging from parents to preeminent researchers and leaders. She is a Medical Writer Certified®, credentialed by the American Medical Writers Association, and received her masters of science in Health Communication from Boston University.
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Post Tags:
- Cardiothoracic Surgery
- The Heart Center
- Posted In:
- Features