A Hidden Epidemic: Parental Incarceration and What To Do When It Affects Your Patients
A Hidden Epidemic: Parental Incarceration and What To Do When It Affects Your Patients https://pediatricsnationwide.org/wp-content/uploads/2019/09/ImpactofParentalIncarcerationInfographic.jpg 1024 512 Andrew Axelson and Samantha Boch, PhD Andrew Axelson and Samantha Boch, PhD https://secure.gravatar.com/avatar/7204da07e8c8363d4e5f1b9e4554b24010dc7b4d87f2ef5a711d8eb890424950?s=96&d=mm&r=g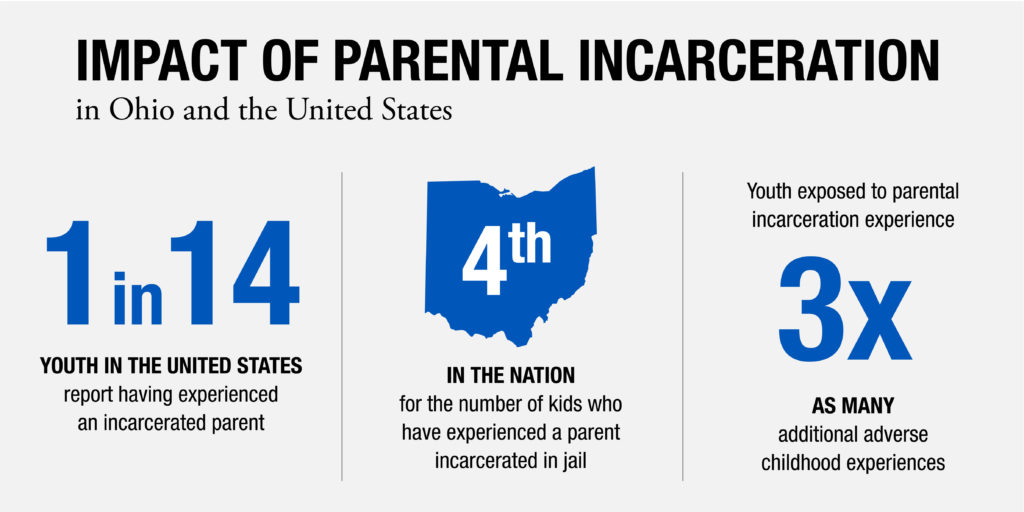
If having an incarcerated parent was classified as a chronic health condition, it would be the second most prevalent chronic condition in the United States for children under the age of 18 – just behind asthma. In fact, the percentage of American youth with an incarcerated parent is about 10 times higher than the percentage of youth diagnosed with diabetes.
Over 5.7 million children, or 1 in every 14 youths, in the United States have had a parent incarcerated at some point during their childhood. And nearly 2.7 million children currently have a parent in jail or prison.
What are the effects of having an incarcerated parent?
Children with incarcerated parents can face tremendous challenges due to the associated economic strain, household churning and instability, and trauma that parental-child separation by incarceration often brings.
Children or young adults who have had an incarcerated parent are more likely to have educational, economic, mental and physical health problems than those unexposed. Parental incarceration has been classified as a particularly stigmatizing Adverse Childhood Experience (ACE), disproportionately impacting children of color and children in poverty.
While the exposure to parental incarceration is often included in ACEs checklists, the experience is rarely solely investigated. Despite new research indicating that these children experience up to three times as many additional ACEs, children exposed to parent incarceration are largely left out of national conversations and political debates surrounding mass incarceration. For these reasons, little research is focused on the differential and contextual impacts of household incarceration (e.g., understanding the difference between parents detained in privately operated facility vs. state/federally operated facility, the frequency of incarceration, prison vs. jail, non-violent offense vs. violent offense, mother vs. father incarceration, sibling vs grandparent incarceration).
While parental incarceration’s effects vary by child, the evidence available points to potential behavioral, emotional and attachment challenges to healthy development. It is also important to note that despite the numerous and unique challenges facing children of incarcerated parents, many children are resilient, rising above multitude barriers to achieve great success.
How can health care providers help?
Understanding and supporting these children and their caregivers through each phase of incarceration (upon arrest, through incarceration and after release) and designing appropriate ways to screen, track and support these families would minimize associated negative impacts.
Yet, no such coordinated system exists.
Because incarceration can be a driver of housing stability, food security, transportation and income, parental incarceration or mass incarceration should be viewed as an important social determinant of health. Connecting and referring these families to mental health and coordinated social services that address the financial, housing, educational and emotional/behavioral health consequences of household incarceration would give affected children much needed access to care and stability.
For youth service providers and teachers, use inclusive familial language and be mindful of the potential barriers of obtaining parental consent to access educational supports (e.g., Individualized Education Program, or IEP) and other school related functions/activities.
Since many of these children have little home stability in their lives and face a fragmented social services system, it is crucial that clinicians make themselves aware of existing Nationwide Children’s community-based resources for at risk youth from intensive home-based treatments and group therapies to school-based programs available to support at risk youth in school, at home, and in the community.
If the child has witnessed violence (e.g. including the witnessing of a traumatic arrest of a parent within the home), referrals to the Center for Family Safety and Healing are also highly encouraged.
Other incarceration-specific resources include:
- Amachi Program: Mentoring for Children with Incarcerated Parents through Big Brothers Big Sisters.
- Sesame Street in Communities – Coping with Incarceration, which provides advice to caregivers and age-appropriate materials for younger children (aged 2-5 years) that introduce the subject of incarceration.
- Unlocking Futures, a Columbus-based organization providing support to families raising children with an incarcerated parent/parental figure using the evidenced-based curriculum, Creating Lasting Family Connections.
- Tip Sheet for Incarcerated Parents: Planning for a Visit from Your Child/Children, which includes age specific guidance and advice for caregivers.
- San Francisco Children of Incarcerated Parents Partnership (SFCIPP), a coalition of those who work with or are concerned about children of incarcerated parents and their families.
- Tips to Support Children When a Parent is in Prison, from the American Academy of Pediatrics Healthy Living blog.
In addition, less than half of the parents in state prisons reported receiving any visits from any of their children. This is unsurprising, as a recent examination of all 50 state’s published correctional visitation and family programming policies conducted at Nationwide Children’s Hospital found vast inconsistencies between states and even between facilities within the same state.
To support parent-child relationships during parental incarceration, consistent, transparent and family-friendly visitation policies and parent education programs that can allow children to have contact with their parent in a positive way are essential. Transportation services and preparing the child with visit expectations and associated safety plans on what to expect, are also encouraged.
The lack of contact between incarcerated parents and their families can lead to additional trauma in children and greater difficulties during the re-entry process. Some states and facilities have already established family-friendly visitation centers and programming in prisons, and it is time to expand these services nationwide.
Similar to the work being done through Nationwide Children’s On Our Sleeves initiative to reduce stigmas surrounding mental health, we should also work to support children by reducing stigmas the stigma of having an incarcerated parent, a part of many children’s lives that is out of their control.
In addition to recognizing the effects of parental incarceration and treating it as a unique childhood experience when working directly with patients, advocating for sentencing and mental health reforms in the prison and child welfare systems could bring about much needed positive change for numerous families in Ohio and beyond.
Health care providers and hospital staff have a unique opportunity and position to advocate on behalf of patients, and children affected by parental incarceration deserve better than what the system designed to protect them currently has to offer.
If you are interested in helping support children of incarcerated parents through advocacy, research or staff education, please reach out to Dr. Samantha Boch at Samantha.boch@nationwidechildrens.org.
About the author
-
Samantha Boch, PhDhttps://pediatricsnationwide.org/author/samantha-boch-phd/
- Posted In:
- Features