In Sight: Two Stage Surgery for Epilepsy
In Sight: Two Stage Surgery for Epilepsy https://pediatricsnationwide.org/wp-content/themes/corpus/images/empty/thumbnail.jpg 150 150 Abbie Miller Abbie Miller https://pediatricsnationwide.org/wp-content/uploads/2023/05/051023BT016-Abbie-Crop.jpgSurgery proves to be a viable option for patients with medically refractory epilepsy.
Childhood onset epilepsy affects 1 percent of children worldwide. About 25 to 30 percent of these patients will have medically refractory epilepsy, continuing to have seizures despite using two or more antiseizure medications. Options for this group of patients include intercranial epilepsy surgery, Vagus nerve stimulator (VNS) insertion, Ketogenic diet and drug trials. It is increasingly recognized that epilepsy surgery may dramatically improve the quality of life for these children in some cases and is the only potentially curative option.
Single or Two Stage Epilepsy Surgery
Single stage surgery is performed if imaging and phase 1 data demonstrate concordant findings suggestions lesional epilepsy. It involves resection of the lesion and electrocorticography to ensure all abnormal tissue is removed. Alternatively, diffuse pathology affecting a cerebral hemisphere may warrant hemispherectomy/hemispherotomy. Two stage surgery is performed when phase 1 monitoring contains discordant data or inadequately localizes the epileptigenic zone. This approach allows identification of the epipleptigenic zone, potential adjacent areas of abnormal electrical activity and nearby eloquent functional areas of the brain. Eloquent areas of cortex are localized by cortical stimulation mapping.
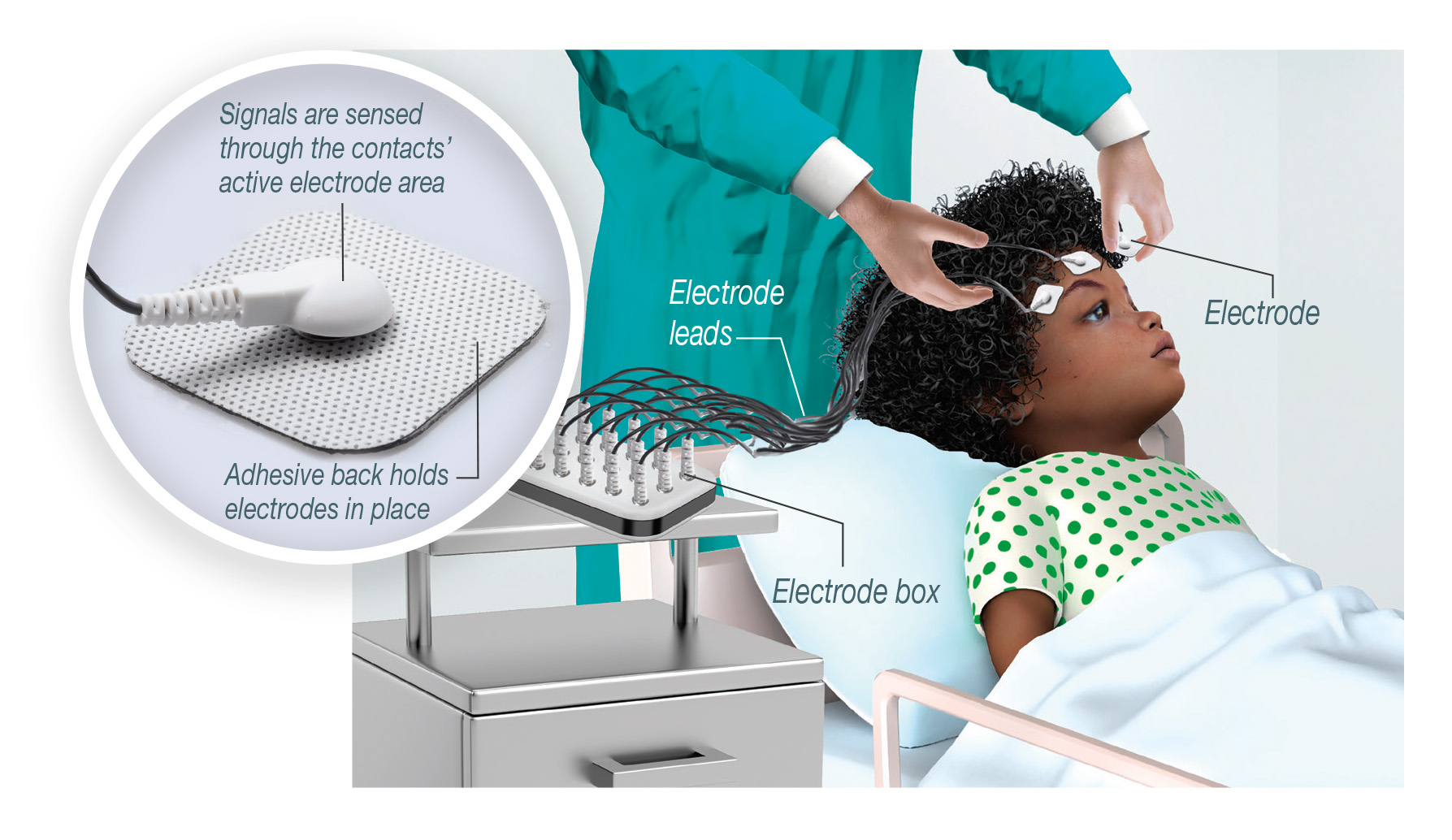
Phase 1 Monitoring
Phase 1 is an extensive presurgical workup that helps the neurologist localize the seizures and determine the patient’s candidacy for epilepsy surgery. This involves multiple-day inpatient admission, prolonged video EEG and intended observation of at least three typical seizures. The patient also undergoes imaging sequences including positron emission tomography (PET), single photon emission computed tomography (SPECT) and epilepsy protocol MRI, in addition to outpatient neuropsychology testing. Potential surgical candidates and all of their clinical and radiographic data are discussed thoroughly at the weekly Epilepsy Surgery Conference. Depending on the results from the Epilepsy Surgery Conference, single stage epilepsy surgery, two stage epilepsy surgery, or palliative surgical options (corpus callosotomy or VNS insertion) may be offered.
Stage 1 Surgery
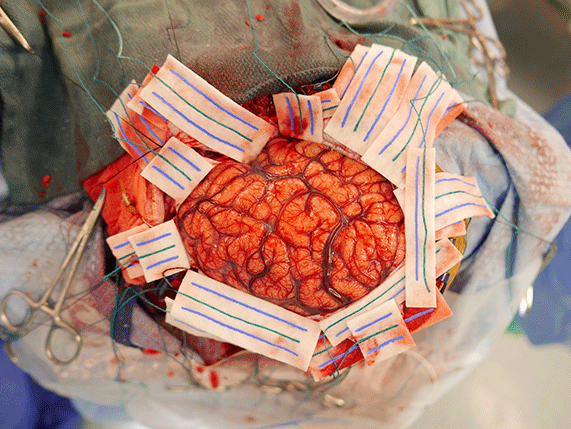
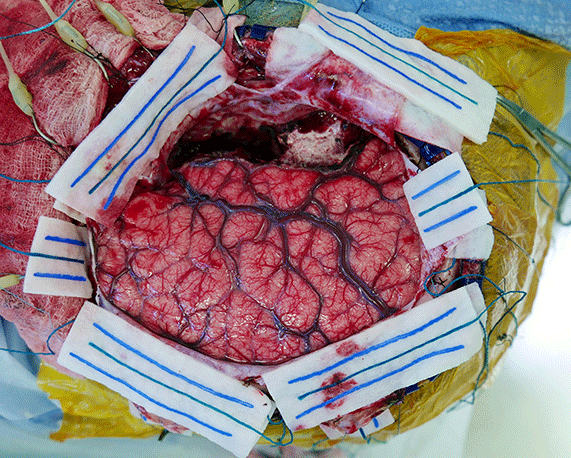
During stage 1 surgery, craniotomy and dural opening allow exposure of the cerebral cortex. Working in collaboration, the neurosurgery and neurology teams identify sites of coverage and access for subdrual grids, strips and/or depth electrodes. Intraoperative electrocorticography confirms adequate placement and signals of intracranial EEG electrodes. The electrodes are safely secured in place as the dura is subsequently
During stage 1 surgery, craniotomy and dural opening allow exposure of the cerebral cortex. Working in collaboration, the neurosurgery and neurology teams identify sites of coverage and access for subdrual grids, strips and/or depth electrodes. Intraoperative electrocorticography confirms adequate placement and signals of intracranial EEG electrodes. The electrodes are safely secured in place as the dura is subsequently closed.
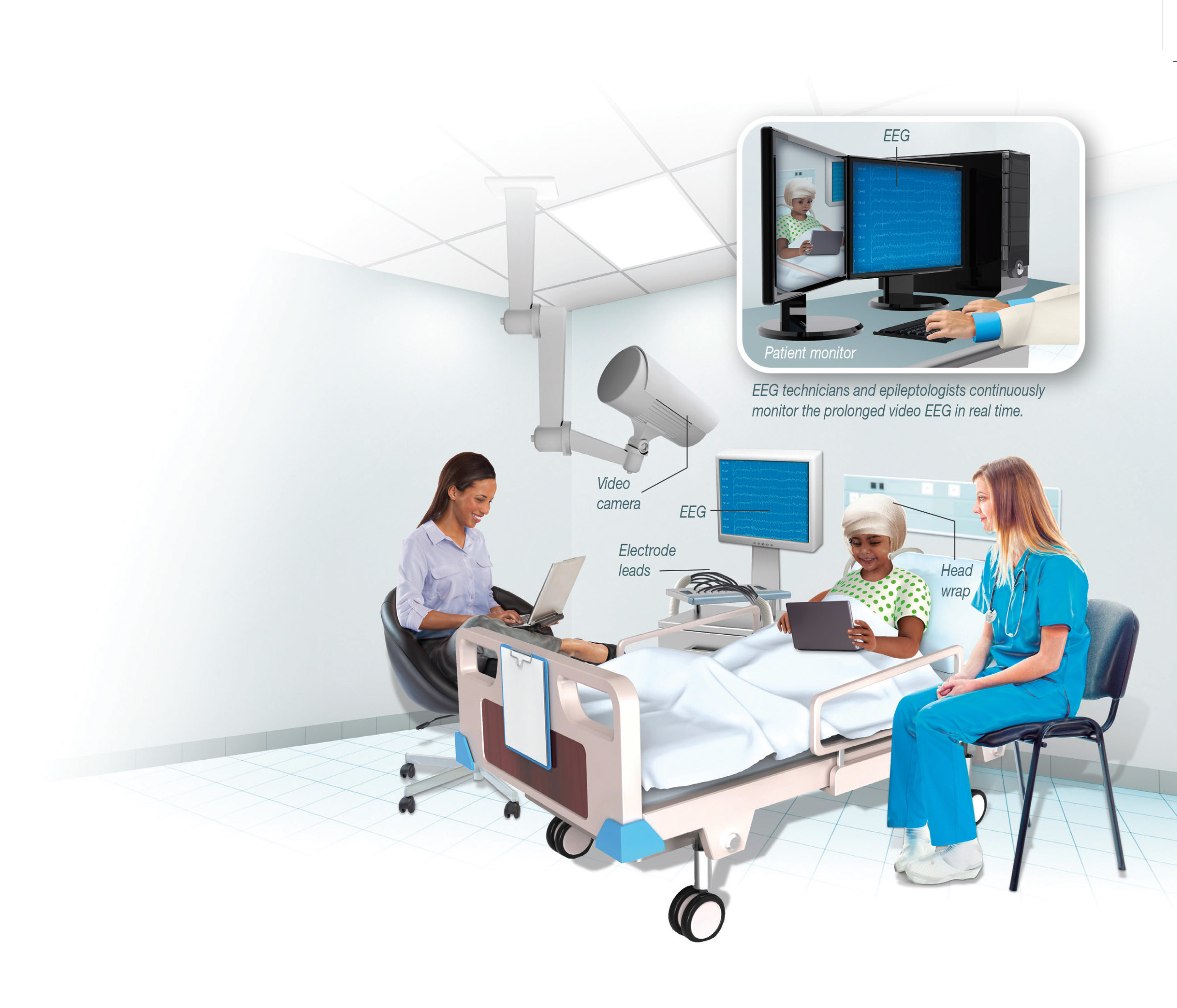
Phase 2 Monitoring
During phase 2 monitoring, continuous, long-term intracranial EEG is monitored for approximately one week to identify abnormal electrical signals before and during seizures. Frequently, antiepileptic medications are weaned to help capture typical seizure activity (at least three events). Near the conclusion of phase 2 monitoring, corticostimulation mapping may identify eloquent functional areas that will help surgical planning. Additional discussion during the Epilepsy Surgical Conference solidifies the surgical plan.
Stage 2 Surgery
Stage 2 surgery typically involves grid-based resection of the epileptigenic zone with careful preservation of adjacent eloquent functional areas. Intraoperative electrocorticography confirms the absence of any residual abnormal electrical activity or identifies additional sites requiring resection. Post operative recovery Following surgery, patients are monitored closely in the pediatric intensive care unit. Once stable, they are transferred to the neurosurgery floor for further recovery. Often patients are discharged to home. However, if needed, transfer to Inpatient Rehabilitation allows for prolonged recovery.
A Patient Perspective: Stopping Gaige’s Seizures
If he stayed up late, Gaige had a seizure. When he got too excited about an upcoming family event, the arrival of Christmas or his birthday, he had a seizure. If he exerted himself while playing basketball, he had a seizure. Read how the epilepsy surgery team at Nationwide Children’s used two stage epilepsy surgery to help.
Graphic: Christina Ullman, Ullman Design
Sources: Jonathan A. Pindrik, MD, pediatric neurosurgeon, Nationwide Children’s Satyanarayana Gedela, MD, pediatric neurologist, Nationwide Children’s
About the author
Abbie (Roth) Miller, MS, MWC, is a passionate communicator of science. As the manager of medical and science content at Nationwide Children’s Hospital, she shares stories about innovative research and discovery with audiences ranging from parents to preeminent researchers and leaders. She is a Medical Writer Certified®, credentialed by the American Medical Writers Association, and received her masters of science in Health Communication from Boston University.
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Abbie Millerhttps://pediatricsnationwide.org/author/abbie-miller/
- Post Tags:
- Epilepsy
- Neurology
- Neurosurgery







