Microsurgery for Acute Flaccid Myelitis: Personalized Approach Leads to Remarkable Recoveries
Microsurgery for Acute Flaccid Myelitis: Personalized Approach Leads to Remarkable Recoveries https://pediatricsnationwide.org/wp-content/uploads/2021/10/AFM-1024x440.jpg 1024 440 Lauren Dembeck Lauren Dembeck https://pediatricsnationwide.org/wp-content/uploads/2021/03/Dembeck_headshot.gif
Children from around the world are coming to Nationwide Children’s for specialized care for AFM with lower extremity involvement. Dr. Amy Moore invented many of the procedures that are leading to remarkable recoveries for these patients.
After an ordinary cold, most people continue with life as usual; however, in some rare cases, a previously healthy child can go from running and playing one day to being unable to walk the next, experiencing rapid paralysis within days or sometimes hours of being sick. This uncommon, polio-like condition is termed acute flaccid myelitis (AFM). It predominantly affects children and is characterized by sudden muscle weakness in the arms and/or legs, which can sometimes turn into permanent paralysis.
Since 2014, cases of AFM have been increasing, with peaks occurring every two years. According to the Centers for Disease Control, 661 cases have been confirmed. In most cases, children with AFM had a cold or fever in the days prior to paralysis. Thus, researchers believe AFM may be caused by a common seasonal virus.
Children with AFM have what appears to be viral-or inflammation-induced damage to the nerves of the spinal cord, including those that control muscles in the arms and legs. While some of these children are able to recover by following activity-based rehabilitation programs, a small percentage have little recovery or see their progress plateau.
These patients and their families are finding hope in a specialized nerve transfer surgery developed by Amy Moore, MD, a plastic and reconstructive surgeon at The Ohio State University Wexner Medical Center and Nationwide Children’s Hospital.
In 2016, the first cohort of children with AFM were brought in for surgical treatment of the paralysis, recounts Dr. Moore.
I work on adults and children to restore motion with nerve transfer, often following trauma or cancer,” says Dr. Moore. “My colleagues who knew I was doing nerve transfers in the lower extremities asked if I would consider seeing these children who could not walk. It was a leap of faith for me and for the parents. When I was in the process of creating these nerve transfers, they trusted me to make this leap of innovation with their child.
– Amy Moore, MD, plastic and reconstructive surgeon at The Ohio State University Wexner Medical Center and Nationwide Children’s Hospital
NERVE TRANSFER
Nerve transfer techniques to restore function in the upper extremities were refined in the late 1990s and early 2000s. These often involve the brachial plexus, a group of nerves that originates in the spinal cord at the neck and controls the movement and feeling to the hand, wrist, elbow and shoulder. Dr. Moore recognized the potential to creatively adapt these techniques to the nerves in the trunk and lower extremities to restore function, including hip stability and leg movement.
During her tenure at Washington University School of Medicine in St. Louis, Missouri, between 2004 and 2011, Dr. Moore pioneered a collection of microsurgical techniques for the lower extremities of children with AFM and recently published details of her approach in the journal of Plastic and Reconstructive Surgery – Global Open.
In 2018 Dr. Moore saw 78% of the estimated potential surgical candidates with AFM. She hopes that publication of the techniques will encourage more surgeons to offer this treatment to patients with AFM and to spread the word to parents that there may be options to further improve the muscle function of children’s paralyzed limbs.
“The lower extremities and the nerves that power them are no different than those in the upper extremities. A nerve is a nerve,” says Dr. Moore. “In nerve transfer, we are using a nerve that is working from a muscle of redundant function or one of less importance. We cut that nerve, move it, and rewire it to a nerve that powers a muscle of more important function.”
Dr. Moore suggests the nerve that allows us to wiggle our toes as an example. “We don’t need to wiggle our toes if we can’t stand.” The surgery works by bypassing the injury in the spinal cord and harnessing the ability of the peripheral nerves to regenerate and connect with the target muscle of greater importance, capitalizing on the brain’s plasticity and ability to relearn the neural pathway. In this example, rerouting the portion of the sciatic nerve that controls the toes to the nerve that controls the gluteal muscle, restoring hip stability.
Dr. Moore and colleagues uses a hierarchy for lower limb recovery goals with hip stabilization at the top of the list, followed by knee extension, then knee flexion. In addition to the restoration of gluteal nerve function using the sciatic nerve, the surgeries may also include splicing of donor nerves that control the sartorius (a long muscle that connects the hip and knee), the obturator (a short muscle connecting the femur and pelvis), and the abdominal muscles to the nerves of the femur and/or hamstrings to restore leg movement and, possibly, the ability to walk again.
To be able to help kids walk again, that’s really something incredible. Our collaboration has fostered the growth of this subspecialty at Nationwide Children’s, and these novel techniques complemented our existing repertoire of techniques and principles used for brachial plexus injuries and traumatic nerve injuries. Offering all of these techniques within one center is unusual, nationally and globally.
– Kim Bjorklund, MD, director of the Brachial Plexus Program at Nationwide Children’s Hospital
Together with physical medicine and rehabilitation specialists, the surgeons conduct a detailed physical examination to determine surgical candidacy — which nerves to reroute to where, depending on the availability of functional nerves. “It’s about being familiar with the anatomy and the topography of the nerves,” says Dr. Moore.
“The difficulty with AFM is that it is very asymmetric. The children do not present with a typical pattern of paralysis. Every child that we’ve seen has been different,” says Nationwide Children’s Physical Medicine and Rehabilitation physician Wilawan Nopkhun, MD, who works with the surgeons as well as with the social workers, physical therapists, and nursing team to plan and execute the children’s rehabilitation plan. “We have to see exactly how they are functioning — all their limbs and their whole body — to determine the donor nerves and the recipient muscles. It’s a combination of where can we take from in order to maximize and optimize their functional recovery.”
“We are seeing success in these kids. They are exposed to hours of therapy for incremental improvements in function,” adds Dr. Moore. “This is really an inspiring group of patients and parents that I feel so privileged to care for. They are the epitome of what hope should be.”
All the patients with AFM from the 2016 cohort have reported improved function after their nerve transfer surgeries. Among those who underwent the surgery for restoration of gluteal function, four of five patients transitioned from using a wheelchair to walking with assistive devices, while children who could walk with assistive devices prior to surgery now have increased endurance and can walk longer distances.
BUILDING AND BROADENING EXPERTISE
In 2019, Kim Bjorklund, MD, director of the Brachial Plexus Program at Nationwide Children’s, started learning the ins and outs of the nerve transfer techniques for the lower extremities from Dr. Moore. The two physicians now perform surgery side-by-side on the same patient, shortening patients’ time in surgery, improving safety, and promoting a uniform standard of care.
“To be able to help kids walk again, that’s really something incredible,” says Dr. Bjorklund, who is also a clinical assistant professor at The Ohio State University. “Our collaboration has fostered the growth of this subspecialty at Nationwide Children’s, and these novel techniques complemented our existing repertoire of techniques and principles used for brachial plexus injuries and traumatic nerve injuries. Offering all of these techniques within one center is unusual, nationally and globally.”
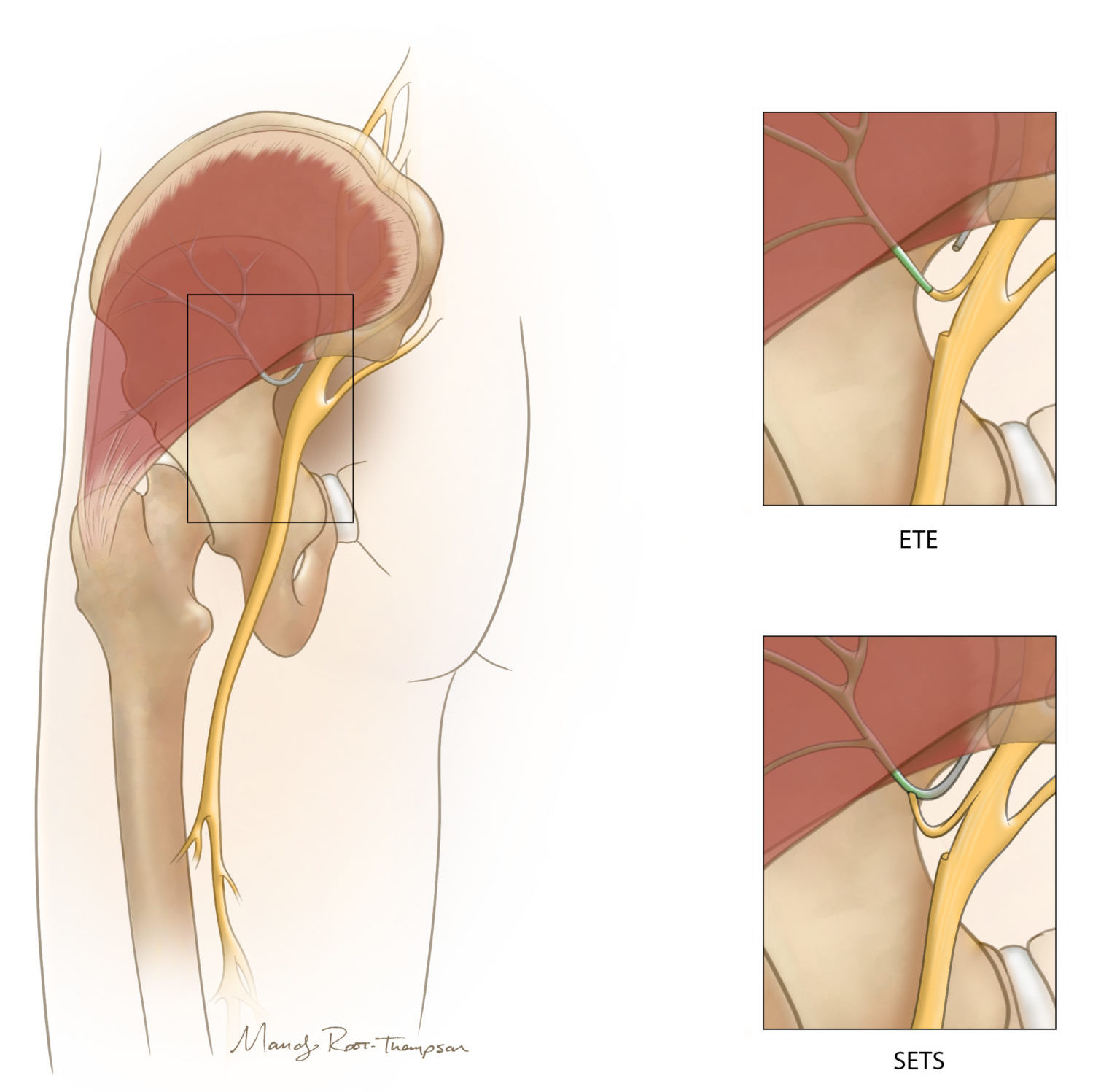
Lower Extremity Nerve Transfer
Microsurgical nerve reconstruction techniques can address functional deficits in the lower extremities of patients with AFM or other nerve disorders. In this example, the patient’s superior gluteal nerve is dysfunctional (indicated in gray). Hip stabilization and restoration of the ability to stand and shift weight can be achieved by transferring a redundant fascicle from the sciatic nerve to the superior gluteal nerve via an end-to-end nerve transfer (upper box) or supercharge end-to-side nerve transfer (lower box). Due to unpredictability in nerve injury patterns and the needs of each patient, a variety of donor and recipient nerves may be used in surgery.
Nationwide Children’s is now developing a comprehensive care center for treating children with a variety of nerve conditions. “Peripheral nerve surgery in general is broad and has a lot of applications to improve function and quality of life for patients,” says Dr. Bjorklund.
In addition to brachial plexus injuries, AFM, and trauma-related injuries, the team is treating patients with a number of other nerve conditions, including those arising from other surgeries, following cancer treatment, and after amputations. For example, the surgeons are able to treat phantom limb pain or ghost pain, a well-known phenomenon associated with amputation. “We perform a procedure called targeted muscle reinnervation, which not only helps with the pain but also improves patients’ function, when using a prosthetic,” explains Dr. Bjorklund.
As a comprehensive care center, multiple physicians in other disciplines, including neurosurgery, orthopedic surgery, internal medicine, general pediatrics, and physical medicine and rehabilitation, will care for patients during and after their nerve surgery.
“After now working with patients with nerve conditions for years, we see that they often have other health issues, such as spinal issues from their lack of muscles, leg length discrepancies, and gastrointestinal issues,” explains Dr. Moore.
Additionally, an early referral is key, says Dr. Nopkhun, “Conducting a full assessment early is important because we typically have limited windows of time where we can potentially intervene for certain conditions and with an early referral we can potentially offer more treatment options.”
The center will also include both clinical and basic science research along with the clinical practice. “As the program grows, this is something that I think is going to benefit children all around,” says Dr. Bjorklund.


This article appears in the 2021 Fall/Winter print issue. Download the full issue.
References:
- Centers for Disease Control and Prevention. Acute Flaccid Myelitis (AFM). Accessed July 20, 2021, at: https://www.cdc.gov/acute-flaccid-myelitis/index.html
- Moore AM. Nerve transfers to restore upper extremity function: A paradigm shift. Frontiers in Neurology. 2014 Mar 31;5:40.
- Moore AM, Bettlach CR, Tung TT, West JM, Russo SA. Lower extremity nerve transfers in acute flaccid myelitis patients: A case series. Plastic and Reconstructive Surgery Global Open. 2021 Jul 20;9(7):e3699.
Image credits: Nationwide Children’s
Medical illustrations by Mandy Root-Thompson for Nationwide Children’s Hospital
About the author
Lauren Dembeck, PhD, is a freelance science and medical writer based in New York City. She completed her BS in biology and BA in foreign languages at West Virginia University. Dr. Dembeck studied the genetic basis of natural variation in complex traits for her doctorate in genetics at North Carolina State University. She then conducted postdoctoral research on the formation and regulation of neuronal circuits at the Okinawa Institute of Science and Technology in Japan.
- Lauren Dembeckhttps://pediatricsnationwide.org/author/lauren-dembeck/
- Lauren Dembeckhttps://pediatricsnationwide.org/author/lauren-dembeck/
- Lauren Dembeckhttps://pediatricsnationwide.org/author/lauren-dembeck/
- Lauren Dembeckhttps://pediatricsnationwide.org/author/lauren-dembeck/January 29, 2019
- Posted In:
- Clinical Updates
- Features
- Research







