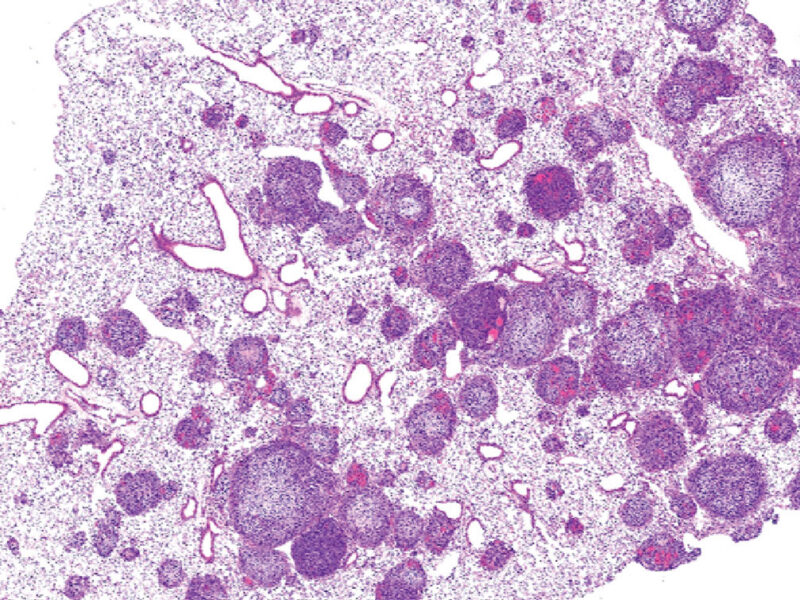
Study Suggests Survivors of Pediatric Brain Tumors Have Altered Connectivity of Key Brain Regions
Study Suggests Survivors of Pediatric Brain Tumors Have Altered Connectivity of Key Brain Regions https://pediatricsnationwide.org/wp-content/uploads/2021/01/AdobeStock_82959563_brain-imaging-for-web-1024x575.gif 1024 575 Lauren Dembeck Lauren Dembeck https://pediatricsnationwide.org/wp-content/uploads/2021/03/Dembeck_headshot.gif
The findings contribute to a scant body of literature on the changes in functional connection within the brain and neurocognitive outcomes in survivors of pediatric brain tumors.
Pediatric brain tumors are the most common solid tumor diagnosis among children in the United States. With advances in treatment, the 5-year survival rate among these children and adolescents has increased to nearly 75%. However, survivors of pediatric brain tumors are susceptible to long-term neurocognitive sequalae.
“People tend to get better more complex cognitive skills as adolescents and young adults. These skills generally involve the coordination of many different regions of the brain that are functionally connected and communicate with each other,” explains Kristen Hoskinson, PhD, neuropsychologist and principal investigator in the Center for Biobehavioral Health at the Abigail Wexner Research Institute at Nationwide Children’s Hospital. “When those connections are impacted by a pediatric brain tumor or its treatment, it can cause a lack of coordination amongst brain regions, potentially lead to poor functional outcomes and cognition and social skills in survivors.”
Dr. Hoskinson and colleagues conducted a pilot study to examine the relationships between neurocognition and activation in regions of the brain that contribute to three major neural networks in survivors of pediatric brain tumors and a cohort of unaffected peers: the central executive network, which shows strong activation during cognitively challenging tasks such as those that involve working memory and decision making; the default mode network, which has been linked to complex neurocognitive processes including memory, social cognition and semantic processing; and the salience network, which is important for modulating shifts between the two other networks.
The researchers hypothesized survivors would have lower within-network connectivity compared with their peers. They also hypothesized brain-based differences in the survivors would be associated with lower performance on cognitive assessments, indicating neurocognitive deficits.
The study was spearheaded by Safiyah Seck, who was volunteering in Dr. Hoskinson’s lab during high school and is now an undergraduate student at Stanford University. Seck and the team used resting state functional magnetic resonance imaging (fMRI) to map the of connectivity among brain regions. fMRI reveals which regions of the brain coactivate and can allow researchers to draw links between differences in the coactivation of brain regions and abnormalities in behavior or cognition.
The study included 13 survivors of pediatric brain tumors (9 boys and 4 girls, with a mean age, of 12.76 years) and 10 healthy children (6 boys and 4 girls, with a mean age of 12.70 years). All participants completed fMRI and assessments of processing speed and executive function.
“In survivors of brain tumors, we found reduced connectivity among brain regions that comprise the salience network, which acts like an on-off switch for the two other networks, and greater connectivity among those comprising the default mode network. When the brains of these children are not able disengage the default mode network to turn on the central executive network, it can contribute to difficulties with cognitively challenging tasks,” explains Dr. Hoskinson.
The researchers found that survivors of pediatric brain tumors demonstrated poorer performance than their peers on measures of processing speed, divided attention, and working memory. They also found that parent ratings of day-to-day executive function did not differ significantly between the groups, but both survivors who underwent only surgical resection and healthy peers were rated by parents as having difficulties in day-to-day behavioral regulation and metacognition that approached or exceeded a full standard deviation above the overall mean.
Using cross-method correlations, the team found that higher central executive network connectivity was associated with poorer parent-rated executive skills. In contrast, they found that increased salience network and default mode network connectivity were associated with better task performance and parent-rated executive skills, suggesting that survivors of pediatric brain tumors may have an adaptive pattern of hyperconnectivity within the brain.
“By knowing certain characteristics of a diagnosis or the type of treatment, we can provide enhanced surveillance for survivors at risk of poor neurocognitive outcomes,” says Dr. Hoskinson. “We’re identifying skill sets that these kids are more likely to have difficulty with, so when necessary, we can target aspects that may be malleable to interventions, such as cognitive and accommodative skills training, school accommodations, behavior management, and psychosocial support.”
Reference
Seck S, Kim YJG, Cunningham WA, Olshefski R, Yeates KO, Vannatta K, Hoskinson KR. Pilot Study of Associations Among Functional Connectivity and Neurocognition in Survivors of Pediatric Brain Tumor and Healthy Peers. Journal of Child Neurology. 2022 Sep 7:8830738221114501. doi: 10.1177/08830738221114501. Epub ahead of print. PMID: 36069044.
Image credit: Adobe Stock
About the author
Lauren Dembeck, PhD, is a freelance science and medical writer based in New York City. She completed her BS in biology and BA in foreign languages at West Virginia University. Dr. Dembeck studied the genetic basis of natural variation in complex traits for her doctorate in genetics at North Carolina State University. She then conducted postdoctoral research on the formation and regulation of neuronal circuits at the Okinawa Institute of Science and Technology in Japan.
- Lauren Dembeckhttps://pediatricsnationwide.org/author/lauren-dembeck/
- Lauren Dembeckhttps://pediatricsnationwide.org/author/lauren-dembeck/
- Lauren Dembeckhttps://pediatricsnationwide.org/author/lauren-dembeck/
- Lauren Dembeckhttps://pediatricsnationwide.org/author/lauren-dembeck/January 29, 2019