Taking on Bronchiolitis in the Age of COVID-19
Taking on Bronchiolitis in the Age of COVID-19 https://pediatricsnationwide.org/wp-content/uploads/2021/01/013019BS2257_c._header-1024x575.jpg 1024 575 Eric Butterman Eric Butterman https://secure.gravatar.com/avatar/8b8fd1d1c3ee8c8b7bb792c663a4bb4f161d83fb0df7c38ac1f8cff3f0468d4f?s=96&d=mm&r=g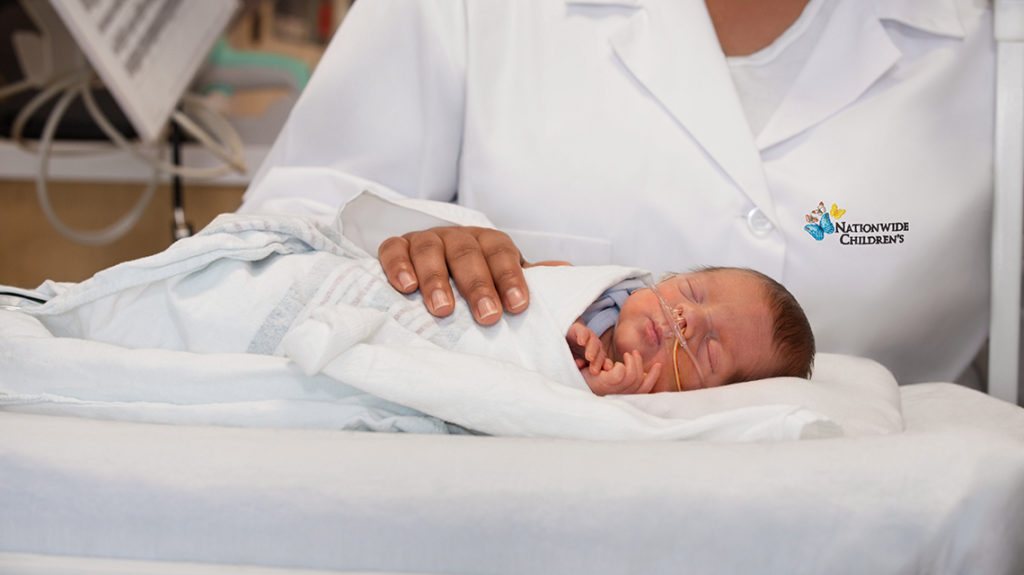
In a recent episode of PediaCast CME, Drs. Asuncion Mejias and Gerd McGwire address the diagnosis and management of bronchiolitis – and special considerations during the COVID-19 pandemic.
Bronchiolitis is the leading cause of hospitalizations for young infants around the world, and in a year with a respiratory pandemic, everyone is a little uneasy about how it could go.
Bronchiolitis is the inflammation of the lower respiratory tract in children younger than 2 years old. It is most commonly caused by respiratory syncytial virus (RSV) but other respiratory viruses such as rhinovirus, influenza and parainfluenza viruses, as well as coronaviruses can also be the cause of bronchiolitis. Data thus far has showed that SARS-CoV-2 is the least likely to trigger bronchiolitis. However, experts say that it is currently to early to known how the novel coronavirus SARS-CoV-2 could influence the 2020-2021 bronchiolitis season.
In early 2020, SARS-CoV-2 appeared in the United States just as the RSV/bronchiolitis season was waning.
“We haven’t really had a substantial SARS-CoV-2 and RSV overlap” but we need to be vigilant and aware that these two viruses may co-circulate, says Asuncion Mejias, MD, infectious disease expert at Nationwide Children’s Hospital.
Diagnosing and Managing Bronchiolitis
Most cases of bronchiolitis are caused by RSV. Although the initial signs and symptoms are similar to that of a common cold, the disease can progress to the lower respiratory tract. These symptoms include:
- Nasal congestion
- Refusal to be fed
- Coughing
- Labored breathing
- Wheezing
- Cyanosis
- Apnea in the very young infant
Diagnosing RSV for children means looking out for symptoms such as a cough, runny nose and difficulty feeding for a few days. Progression from upper to lower respiratory tract involvement occur in about 25% of children with RSV, and in these infants the difficulty breathing progressing over time.
“It can be hard to predict how children will do though,” Dr. Mejias says. “The infection can be restricted to the upper respiratory tract, but RSV has a predilection for young infants, and these patient population are at a higher risk of severe disease because of the lack of maturity of their immune system and also because their airways are smaller. Babies younger than 6 months old are exclusive nose breathers, so when they have a stuffy nose, their breathing is jeopardized much more than for the older infant or child.”
Those hospitalized may need oxygen and possibly even ICU care as eating issues are common, adds Gerd McGwire, MD, pediatric hospitalist.
Typically, diagnosing bronchiolitis is straightforward for the young infant, says Dr. McGwire. There aren’t many differential diagnoses to consider for babies under 1 year old. However, once children reach the 1-to-2-year-old range, physicians should consider recurrent wheezing, a family history of asthma, pertussis or bacterial pneumonia.
In the age of COVID-19, providers and families have a new differential to consider. Many of the symptoms of COVID-19 overlap with bronchiolitis. Which may mean more testing will be required to confirm diagnoses.
“An RVS/flu/COVID rapid test is under development,” says Dr. Mejias. “And that would be extremely helpful this year. Normally, in the outpatient setting confirmatory RSV test are not performed, but this year the implementation of viral testing to rule out COVID and confirm the diagnosis will be important not only for easing the minds of parents and providers, but for patient management.
Reference:
Podcast – Bronchiolitis: Diagnosis, Management, Prevention – PediaCast CME 057I (shared September 16, 2020)
Image credit: Nationwide Children’s
- Post Tags:
- COVID-19
- Critical Care
- General Pediatrics
- Posted In:
- In Brief