Keeping Options Open in Complex Pediatric Nephrolithiasis
Keeping Options Open in Complex Pediatric Nephrolithiasis https://pediatricsnationwide.org/wp-content/uploads/2021/01/Urinary-system-No-Background-kidney-header-1024x575.jpg 1024 575 Lauren Dembeck Lauren Dembeck https://pediatricsnationwide.org/wp-content/uploads/2021/03/Dembeck_headshot.gif- March 01, 2020
- Lauren Dembeck
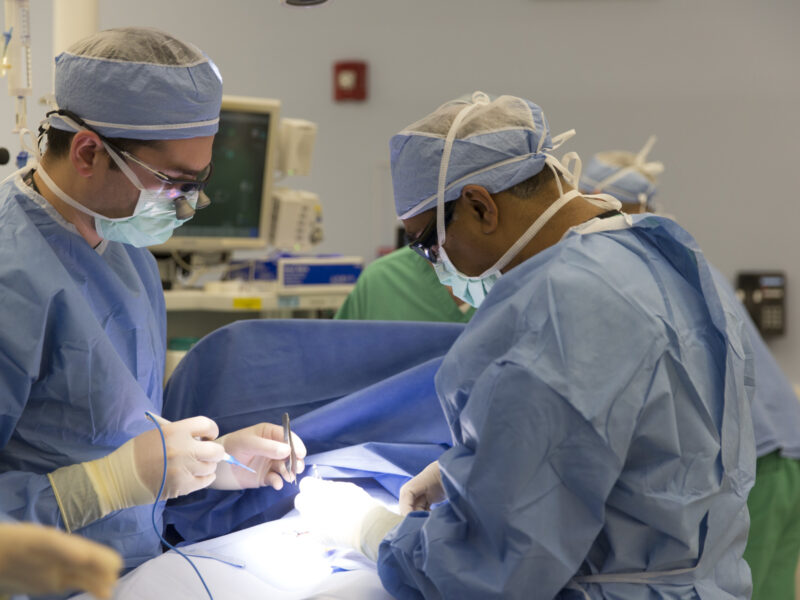
Urologists in the Pediatric Urology Midwest Alliance recently looked at how endoscopic assisted robotic pyelolithotomy could reduce the number of procedures for children with ureteropelvic junction obstruction.
The Pediatric Urology Midwest Alliance (PUMA) recently published a new report demonstrating that endoscopic assisted robotic pyelolithotomy (EARP) is an acceptable treatment option for complex cases of pediatric nephrolithiasis.
The multicenter, collaborative study included a retrospective analysis of all robotic procedures performed at the five PUMA institutions from July 2009 to October 2017 and was published in the Journal of Pediatric Urology.
“Many of these children required an operation to fix anatomic abnormalities or UPJ [ureteropelvic junction] obstruction, and the operation usually opens up the renal pelvis where the stone is. Thus, it’s prudent to be able to, during the same operation, go into the kidney through the opening that you already have and take out any stones; so, you can actually do two procedures at once,” explains study author Daniel DaJusta, MD, pediatric urologist at Nationwide Children’s Hospital, which is one of the PUMA institutions.
Among 26 patients (median age, 12.2 years) who underwent EARP, the investigators found that almost 80% of patients who underwent a concomitant pyeloplasty-pyelolithotomy due to a UPJ obstruction and a stone could have had, according to the current standard of care, a percutaneous nephrolithotomy. However, all of these patients would then require a second procedure to treat the UPJ obstruction. Of those who underwent EARP, 70% required only one procedure to address both problems.
The reasons for EARP were concomitant pyeloplasty (77.8%), altered anatomy precluding other techniques (14.8%) and multiple large stones (7.4%). The median operative dimension of the largest stone was 9.0 mm, and a majority of renal units, either kidneys or ureters, (74.1%) had multiple stones. Stones were usually located in the renal pelvis (33.3%) or lower pole (37.0%) but were also found in the ureter (3.7%) and multiple locations (25.9%).
After EARP, the overall stone-free status was 70.4%. Residuals stones in eight kidneys were managed by ureteroscopy (4), extracorporeal shock wave lithotripsy (2), and percutaneous nephrolithotomy (1), while one was passed spontaneously.
“There are not that many children with a concomitant UPJ or in which we have difficulty accessing the kidneys. Most of us in pediatric urology will have up to a handful of these kids,” says Dr. DaJusta, who is also a clinical associate professor of Urology at The Ohio State University College of Medicine.
That’s why multicenter research collaboratives, such as PUMA, that involve surgeons doing similar procedures who are able to pool data make for stronger, more robust studies, he says. The data is more compelling compared to a report with just a few cases.
“Finding people who are willing to work together towards a common goal, especially towards improving patient care, and building a successful collaboration, isn’t easy because institutions have different guidelines and restrictions about data sharing. But it’s a great idea, and I think it only strengthens the ability to produce stronger, better research,” he adds.
Reference
Roth JD, Gargollo PC, DaJusta DG, Lindgren BW, Noh PH, Rensing AJ, Krambeck AE, Whittam BM, Pediatric Urology Midwest Alliance (P.U.M.A.). Endoscopic-assisted Robotic Pyelolithotomy: A Viable Treatment Option for Complex Pediatric Nephrolithiasis. Journal of Pediatric Urology. 2019 Dec 19[Online ahead of print].
Photo credit: Nationwide Children’s
About the author
Lauren Dembeck, PhD, is a freelance science and medical writer based in New York City. She completed her BS in biology and BA in foreign languages at West Virginia University. Dr. Dembeck studied the genetic basis of natural variation in complex traits for her doctorate in genetics at North Carolina State University. She then conducted postdoctoral research on the formation and regulation of neuronal circuits at the Okinawa Institute of Science and Technology in Japan.
-
Lauren Dembeckhttps://pediatricsnationwide.org/author/lauren-dembeck/
-
Lauren Dembeckhttps://pediatricsnationwide.org/author/lauren-dembeck/
-
Lauren Dembeckhttps://pediatricsnationwide.org/author/lauren-dembeck/
-
Lauren Dembeckhttps://pediatricsnationwide.org/author/lauren-dembeck/January 29, 2019