Robotic Approach to Rare Case Leads to Best Possible Outcome
Robotic Approach to Rare Case Leads to Best Possible Outcome https://pediatricsnationwide.org/wp-content/uploads/2022/11/fLKHq3C0-1024x683.jpeg 1024 683 Emily Siebenmorgen Emily Siebenmorgen https://pediatricsnationwide.org/wp-content/uploads/2023/05/Emily.Siebenmorgen-scaled-e1684876333147.jpg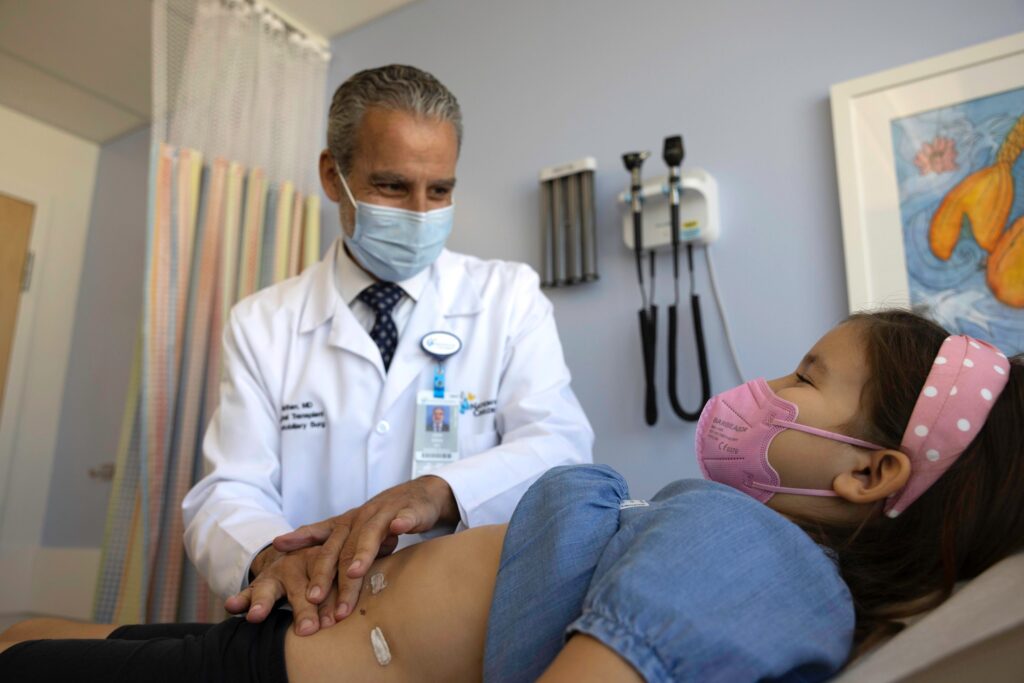
A rare tumor in a child from Greece is resolved by robotic spleen-sparing distal pancreatectomy.
Hospital visits can feel like a foreign experience for anyone, especially so when your hospital is actually in another country. But eight-year-old Evangelia felt especially at home after traveling to Nationwide Children’s Hospital from Greece for her care.
Evangelia’s first episode of severe abdominal pain and illness happened in 2021.
“Back then we thought it was related to a virus,” Evangelia’s father, Nikos, says. “But a year later she had another episode. After that, we went to the hospital and did every exam possible.”
An MRI showed a large, three-centimeter tumor on Evangelia’s pancreas. It was suspected to be benign, but Evangelia needed a distal pancreatectomy to remove it. Because her condition is so rare in children, her family looked abroad to find the best possible care.
“We went through lots of inquiries – first in Greece, and then Europe and the United States,” Nikos says. “We were advised that Dr. Jaimie Nathan is an expert in pancreatic surgeries and an ideal fit because our specific case is very rare. He has the expertise that inspired us to have the operation in Columbus, even if it was far from Greece.”
Children who need a distal pancreatectomy typically have three options for surgery: an open operation, which leaves a larger scar and typically involves more pain and longer healing; a minimally invasive laparoscopic operation, which involves small incisions; or minimally invasive robotic operation, which also involves small incisions. In adults, where pancreatectomies are more common, many operations are laparoscopic or robotic.
A robotic approach to distal pancreatectomy offers some distinct advantages, particularly in pediatric patients. Operating with the robot gives greater dexterity, particularly for navigating in tight corners and spaces. Robotic operations also afford the surgeon a three-dimensional visualization compared to a laparoscopic approach with two-dimensional visualization.
“While it has many advantages, most pediatric surgeons don’t have the experience using robotic surgery for complex distal pancreatectomies, especially in cases where dissecting out the splenic artery and vein are essential to preserving the spleen,” says Jaimie D. Nathan, MD, chief of Pediatric Abdominal Transplant and Hepatopancreatobiliary Surgery at Nationwide Children’s. “Cases like this are extremely rare in the literature, but I’ve had the experience of doing many complex pancreatic and hepatobiliary operations robotically over my career in pediatric surgery.”
The benefits of robotic surgery were important for one of the family’s goals: preserving Evangelia’s spleen. Spleen preservation is an ideal for abdominal surgeries, but it is not always possible. While complications from splenectomy are rare, they may be devastating when they occur.
Dr. Nathan’s approach saved her spleen and successfully removed the pancreatic tumor. Biopsy confirmed that the tumor (solid pseudopapillary neoplasm) was benign, making the operation curative. After her hospitalization, she was able to stay with her family locally until they returned to Greece three weeks after the surgery.
“In our effort to find the best possible care and treatment for our daughter, we were communicating with several hospitals – including three of the top hospitals in the United States,” Evangelia’s mother, Katerina says. “Nationwide Children’s was the best hospital that we’ve visited – it’s fantastic, well-organized. Global Patient Services had such quick responses, we didn’t lose time coordinating her care. We felt so safe and comfortable, and the staff made all the difference.”
About the author
Emily Siebenmorgen is a Science Communication Specialist at Nationwide Children's Hospital with a passion for making research findings accessible. From her time writing at Battelle and AWRI's Center for Injury Research and Policy, she has experience distilling complex topics into simple takeaways for both professional and consumer audiences. Emily earned her BS in Psychology and BA in Strategic Communication from The Ohio State University.
- Emily Siebenmorgenhttps://pediatricsnationwide.org/author/emily-siebenmorgen/
- Emily Siebenmorgenhttps://pediatricsnationwide.org/author/emily-siebenmorgen/
- Emily Siebenmorgenhttps://pediatricsnationwide.org/author/emily-siebenmorgen/September 29, 2022
- Emily Siebenmorgenhttps://pediatricsnationwide.org/author/emily-siebenmorgen/October 17, 2022
- Posted In:
- Patient Story