InSight: A Window to the Heart
InSight: A Window to the Heart https://pediatricsnationwide.org/wp-content/uploads/2015/04/Fontan-with-heart-transparent-header.jpg 720 530 Katie Brind'Amour, PhD, MS, CHES Katie Brind'Amour, PhD, MS, CHES https://pediatricsnationwide.org/wp-content/uploads/2021/03/Katie-B-portrait.gif- April 25, 2015
- Katie Brind'Amour, PhD, MS, CHES
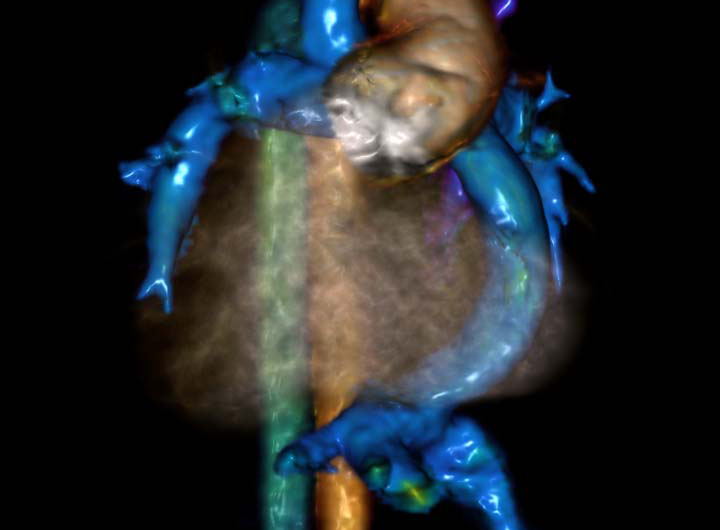
Cardiac MRI for Hypoplastic Left Heart Syndrome
Hypoplastic left heart syndrome (HLHS) is a potentially fatal congenital heart defect affecting blood flow. It requires multiple palliative surgeries, starting within the first week of life. Nationwide Children’s employs a hybrid surgical approach.
Hybrid Stage I (not shown)
Bilateral branch pulmonary bands are placed to restrict blood flow. A stent is placed to augment systemic blood flow, and an atrial septostomy allows improved mixing of the saturated and unsaturated blood. Unlike the standard Norwood procedure, hybrid stage I typically allows discharge within a week or two.
Comprehensive Stage II
This surgery removes the previous stent and bands and surgically enlarges the atrial defect. This stage also includes aortic arch reconstruction and connects the superior vena cava to the pulmonary artery (bidirectional Glenn).
In this 6-month-old patient, cardiac MRK enabled cardiologists to identify three abnormalities: a clot in a portion of the azygous vein, a veno-venous collateral vessel and a kink or narrowing at the point of insertion of the superior vena cava into the right pulmonary artery (bidirectional Glenn), altering the patient’s treatment.
Stage III – Fontan Procedure
The final palliative surgery for patients with single ventricle defects completes the cavo-pulmonary anastomosis (Fontan), which routes blood from the lower part of the body directly to the pulmonary artery.
This image depicts the heart of a 16-year-old patient with situs inversus with dextrocardia, tricuspid atresia and L-transposition of the great arteries who underwent a Fontan procedure and is now more desaturated (blue). Cardiac MRI provided a roadmap for the cardiac catheterization team and enabled a more efficient procedure, which included occlusion of veno-venous collateral vessels and stent placement in the affected portion of the central pulmonary artery.
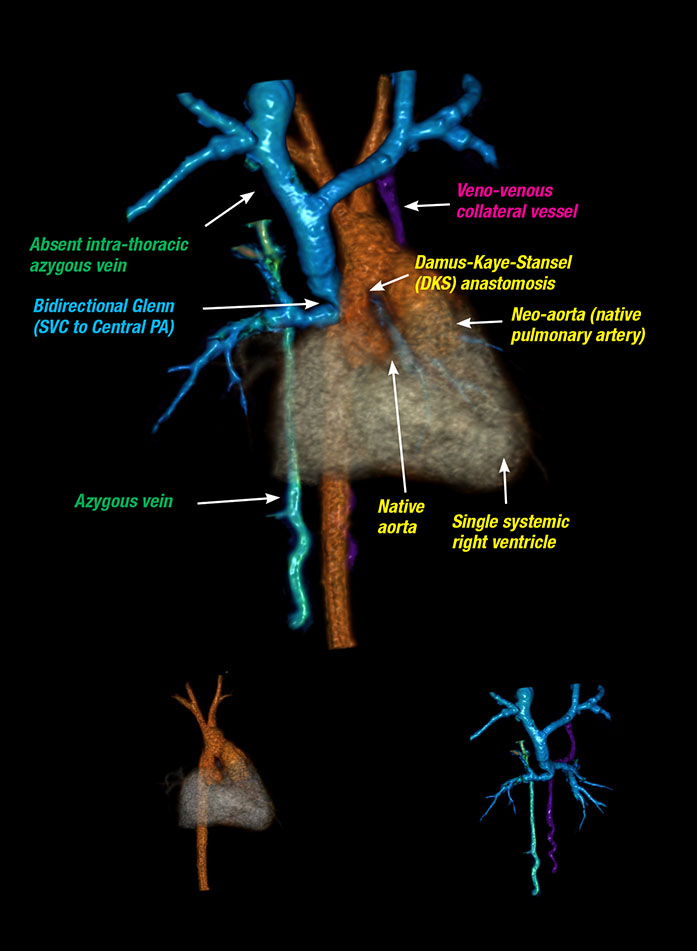
In this 6-month-old patient, cardiac MRI enabled cardiologists to identify three abnormalities, altering the patient’s Comprehensive Stage II HLHS treatment. The imaging technology allows the user to break the image down by system and rotate or color code it for better visibility.
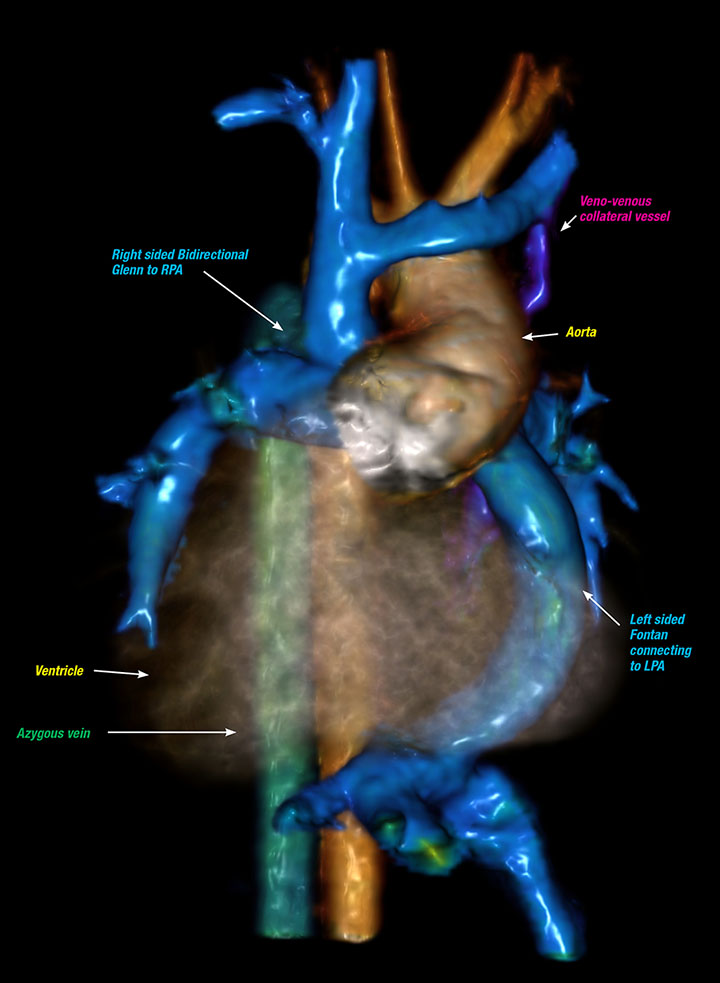
This image depicts the heart of a 16-year-old patient with situs inversus with dextrocardia, tricuspid atresia and L-transposition of the great arteries. Cardiac MRI provided a roadmap for the cardiac catheterization team and enabled a more efficient procedure.
About the author
Katherine (Katie) Brind’Amour is a freelance medical and health science writer based in Pennsylvania. She has written about nearly every therapeutic area for patients, doctors and the general public. Dr. Brind’Amour specializes in health literacy and patient education. She completed her BS and MS degrees in Biology at Arizona State University and her PhD in Health Services Management and Policy at The Ohio State University. She is a Certified Health Education Specialist and is interested in health promotion via health programs and the communication of medical information.
-
Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
-
Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
-
Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 27, 2014
-
Katie Brind'Amour, PhD, MS, CHEShttps://pediatricsnationwide.org/author/katie-brindamour-phd-ms-ches/April 28, 2014
- Posted In:
- Features





